The Treatment That Finally Lifted My Depression After Everything Else Failed
Updated: Jul. 19, 2017
More than 15 million Americans suffer from depression, and more than a third of them don't respond to counseling or antidepressants. Nathalie DeGravel was one of the unlucky ones—until she discovered a novel new therapy.
 Four years ago, Nathalie DeGravel, 48, finally recognized something was horribly wrong with her brain. A human resources coordinator at the time, and living in Los Angeles, she knew that the episodes of rage and crying she battled frequently were much worse than the typical emotions everyone experiences. But her trips to a psychiatrist and prescription medications couldn’t put a dent in the vicious depression she was suffering. Her despair at finding a solution led her to an unconventional new treatment—which ended up saving her life.
Four years ago, Nathalie DeGravel, 48, finally recognized something was horribly wrong with her brain. A human resources coordinator at the time, and living in Los Angeles, she knew that the episodes of rage and crying she battled frequently were much worse than the typical emotions everyone experiences. But her trips to a psychiatrist and prescription medications couldn’t put a dent in the vicious depression she was suffering. Her despair at finding a solution led her to an unconventional new treatment—which ended up saving her life.
Born in Paris, France, DeGravel had always been content with the pleasant life she built in the United States: A husband and two children she enjoyed immensely, a satisfying career, with occasional trips to visit family in Paris. When her symptoms of depression began, they were mild, almost unnoticeable. Over time, however, the mental illness grew in severity to the point she couldn’t even recognize herself, or the life she had worked so hard to build.
“It started with anxiety a few years back, and I would experience rage as well,” says DeGravel. “I shouted and hit objects. At one point, I even emptied the trash can on my husband’s head.” Her feelings eventually caused her to withdraw from those she loved most, creating a sense of confusion and anger that radiated through her family. “I would isolate myself and leave the house for the entire day, not saying where I was. I wouldn’t respond to the phone when I was actually just in a parking lot, listening to music or sleeping in my car,” she recalls. Simple tasks such as showering and taking care of her family became overwhelming. “I cried all the time for no reason,” DeGravel says. “I was lethargic, I would sleep or stay in bed all day long without eating. I progressively became overwhelmed by daily tasks even though I wasn’t working and my youngest child is in high school. Cooking, housekeeping, and grocery shopping would provoke panic attacks.” Here’s what not to say to someone who’s depressed.
As DeGravel’s life began to spiral out of control, her loved ones became tangled in the web of her illness. “My husband had to do his own therapy to understand what happened to me and to cope with the changes at home. He was frustrated, angry, and resentful. Our relationship in general was in constant conflict, and we didn’t have fun together anymore,” she explains. (Dealing with a depressed spouse can be extremely tricky.)
DeGravel found herself focusing solely on doing the unthinkable—ending her own life. She recalls, ” I would think all day and night about how I could kill myself so that it looked like an accident: My husband could get the life insurance money, and my kids would not feel guilty, because it wouldn’t be their fault.” Her career suffered the strain of her illness as well: She ultimately walked away from her job while she struggled to survive each and every day. “When I was working I was unable to concentrate, couldn’t remember what I read or the instructions I was given. I’d miss deadlines, and fall asleep during meetings and at my desk,” she said. During her worst moments, she wondered why her life had taken such a tragic turn. “The first thing I always asked myself was ‘Why? Why me?’ I used to be strong, independent, able to control my emotions, and able to know what I wanted,” she says. “I moved from France to the US and found a job quickly, visited my family regularly, was in good health. I had good friends, I bought a house. I was known for my character: strong, but generous and fair. In short, I was not a weak person, and I accomplished a lot in life. So why me?”
Desperate to regain control over her life, DeGravel sought out the help of a psychiatrist. But repeated attempts at traditional therapy and medication did nothing to ease her symptoms. DeGravel knew she had to think outside the box. “I was online when I saw an advertisement for transcranial magnetic stimulation. I had never heard about it and I was desperate for any solution. I talked to my psychiatrist about it, and he enrolled me in the program at UCLA,” she recalls.
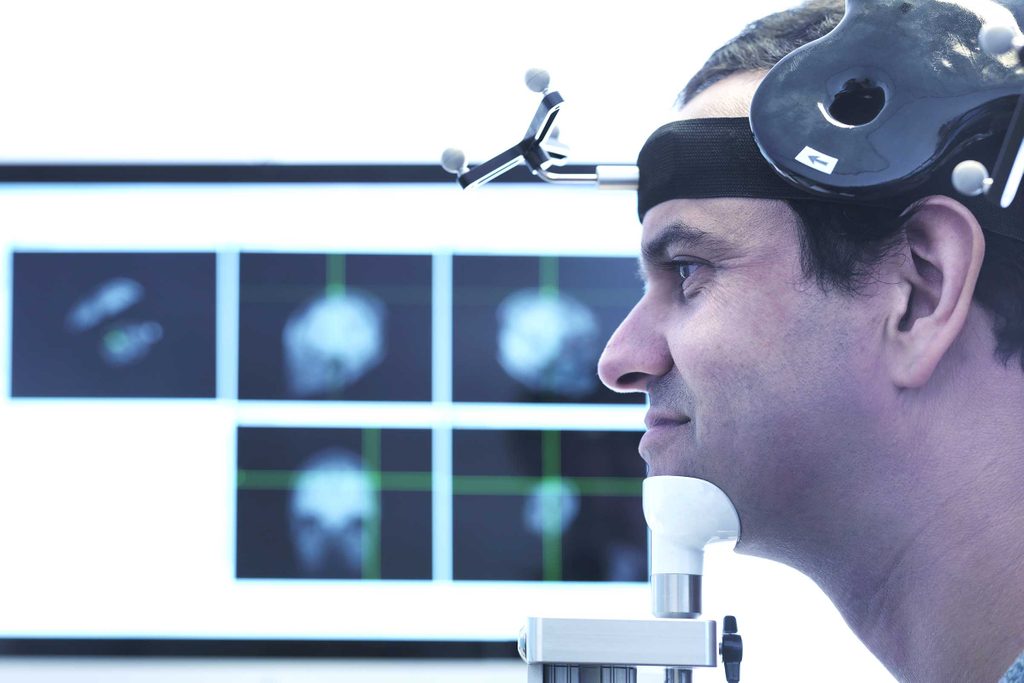 Transcranial magnetic stimulation (TMS) is a recently developed therapy in which magnetic pulses are beamed deep into mood centers in the brain; while no one is sure exactly why the treatment works, the increased neural activity over time—TMS is done several times a week for four to six weeks—seems to rewire the brain, easing depressive symptoms and thoughts. Ian Cook, MD, director of the UCLA Depression Research and Clinic Program where DeGravel received treatment, told the UCLA News Room, “We are actually changing how the brain circuits are arranged, how they talk to each other. The brain is an amazingly changeable organ, and we hope this technology will have use, not just in depression, but for other conditions as well.” The development of the new therapy to treat stubborn depression is an encouraging sign for the 30 percent of people whose symptoms are treatment resistant to other therapies. (TMS is just one of several promising advances in depression treatment.)
Transcranial magnetic stimulation (TMS) is a recently developed therapy in which magnetic pulses are beamed deep into mood centers in the brain; while no one is sure exactly why the treatment works, the increased neural activity over time—TMS is done several times a week for four to six weeks—seems to rewire the brain, easing depressive symptoms and thoughts. Ian Cook, MD, director of the UCLA Depression Research and Clinic Program where DeGravel received treatment, told the UCLA News Room, “We are actually changing how the brain circuits are arranged, how they talk to each other. The brain is an amazingly changeable organ, and we hope this technology will have use, not just in depression, but for other conditions as well.” The development of the new therapy to treat stubborn depression is an encouraging sign for the 30 percent of people whose symptoms are treatment resistant to other therapies. (TMS is just one of several promising advances in depression treatment.)
The FDA-approved treatment requires patients to visit a TMS center. The doctor positions an electromagnetic coil against the patient’s scalp, and then administers magnetic pulses for 30 to 40 minutes. For the most part, the non-invasive treatment is painless, though some patients experience temporary pain at the site or mild headaches. DeGravel’s experience with the treatment was positive: “After about 5 weeks I noticed the treatment had an impact on my symptoms. I felt almost normal. I had control of my emotions, I was socializing again, I wasn’t crying, and I had no suicidal thoughts.” Physically, the procedure was relatively easy to tolerate. She recalls, “When the set-up is finalized the sessions last only about 40 minutes. It’s noisy, but I wear earplugs, and it feels like I have a woodpecker on my head. Some people watch TV during the sessions, but I prefer to check my emails or Facebook.” The new therapy has had such a profound impact on her life that DeGravel hopes others suffering from the same debilitating symptoms will consider the treatment. “I encourage anyone with depression to give TMS a try. I was in their shoes a few months back, and I only regret one thing—not knowing about it earlier!” TMS is an option for patients who, like DeGravel, have failed to find relief with counseling and drug therapy.
