
“I gave up gluten, meat, and chocolate”
Endometriosis is a condition in which tissue similar to that which lines a woman’s uterus goes rogue, growing in places outside of the uterus and causing scar tissue, pain, heavy bleeding, and irregular menstrual cycles. So far, there’s no one set cure; some women suffer for years, trying everything they can to deal with the worsening symptoms. Mary Smith, of Lodi, CA, says she found relief in following an anti-inflammatory endometriosis diet. “You basically remove everything lovely from your diet: All gluten, pork products, dairy, chocolate, coffee, and any meat that has added hormones,” she explains. “I was never 100 percent symptom-free, but I went from having a period every 10 days and needing prescription painkillers for the cramps to a 24-day cycle and ibuprofen. I hated the thought of such a severe diet change but after my health improved so much, you couldn’t pay me to eat bread again!” For a glimpse of what it’s like to live with this condition, don’t miss this woman’s harrowing battle with endometriosis.
“I gave up an ovary”
While bleeding, pain, and irregular periods are the most common symptoms of endometriosis, the condition can also cause fatigue, painful sex, depression, pelvic pressure, bloating, gastrointestinal problems, and cramping. Many of these symptoms are dependent on where the endometrial tissue is growing and what organs it affects, which means treatments are targeted to individual symptoms. For Elizabeth D., of Quantico, VA, it meant having one of her ovaries, the organ most covered in tissue, removed. Afterwards, she says, she went on long-term hormonal birth control to keep new tissue from growing. “In doing this, I have kept my period almost entirely at bay for years,” she says. “I’m so happy to have found what works for me!”
“I’m on birth control pills for life”
Infertility or problems getting pregnant is a common and devastating side effect of endometriosis. In fact, it’s often what leads a woman to finally getting a diagnosis—which is exactly what happened to Melissa O., of Prior Lake, MN. She was diagnosed with endometriosis after suffering an ectopic pregnancy. “I had laparoscopic surgery to have some of the scar tissue removed. After that my doctor put me on birth control pills to help keep the endo from growing back,” she says. When she decided to start a family, she quit the pills to became pregnant, eventually giving birth to a healthy son. And delaying going back on the pills was a big mistake, she says. “I know that I’ve had regrowth based on how painful my periods became over the last few years—on my worst days I can’t move, eat, or drink,” she says. “I’ve been back on the pill for about six months and have almost no pain now—I’m so happy.” P.S. An irregular period doesn’t always mean endometriosis; it can also be one of the 11 signs you’re in perimenopause.

“I use a mix of Western and Eastern medicines”
When it comes to treating her endometriosis, April Olshavsky, of Phoenix, AZ, isn’t afraid to try new things. She tried the medical route, having five surgeries including a hysterectomy. But she still hadn’t found total relief, so she began seeing an advanced pelvic physician and tried a cocktail of homeopathic and herbal treatments. “For me, it isn’t just one thing that helps, but a combination of many trial-and-error options. I’ve had the most success with doing a year of pelvic floor therapy, dry-needling, cupping, heat packs, and seeing the pelvic physician,” she explains. “Part of doing a whole-body treatment plan means that I’ve had to change the way I plan my day, from eating to sleeping. I learned how to watch for signals an attack is coming on, and use CBD oil, kratom, and medical marijuana to manage pain. I’ve also recently been prescribed Bentyl for secondary symptom management and had good results, so far.”
“I got monthly hormone injections”
For women who still want to have children, their surgical options may be limited. Doctors can try medications to temporarily suppress the hormones that can spur endometrial growth. That was the route Kara Phillips, of Superior, CO, chose before having her four children. “I got Lupron injections for six months in my early 20s, which basically put me into temporary menopause,” she says. “They stopped my symptoms until I was ready to get pregnant, and as a happy side effect, the injections also improved my fertility.” After her family was complete, Kara opted for a hysterectomy. Not all hysterectomies remove the entire uterus—that’s just one of the hysterectomy myths women can safely ignore.
“I had my uterus and ovaries removed”
The condition hits about 1 in 10 women during their childbearing years, according to Endometriosis.org. One of these, Susan Schear, of Scottsdale, AZ, suffered for decades with severe bleeding, cramping, and pain before she opted for removal. “I’d had two previous surgeries and the endo would just come back with a vengeance, even on birth control. My life was consistently disrupted by pain. Sex hurt. Peeing hurt. Sitting hurt. I even had to have an appendectomy from having my appendix covered in endometrial tissue. The final straw was getting a CAT scan and it showed my uterus was as big as if I were 16 weeks pregnant because it was filled with fibroids and adenomyosis. It had to go,” she says. She had a complete hysterectomy, removing both the uterus and her ovaries, in 2018. “Now, I want to run down the street screaming to everyone how fabulous life is without my uterus and ovaries!” she says. Endometriosis is one of the 11 sneaky reasons for a missed period.
“I had the lining of my uterus lasered off”
Ablation therapy—an outpatient surgery where a tool is used to remove the lining of the uterus—is one of the most common treatments for endometriosis. Surgeons can do the procedure several different ways, including using extreme cold, heated fluids, microwave energy, or high-energy radio frequencies, according to the Mayo Clinic. It’s popular because it requires very little downtime and can stop or lighten periods for months or even years. It can’t treat existing tissue outside the uterus, but it can help mitigate the painful periods that come with endometriosis—and that’s the reason Kim DeBerge, of Minneapolis, MN, chose it. “I had two ablations several years apart,” she says. “My only other option was to have a complete hysterectomy, so the ablations kept me from having to go through full-blown menopause at a very young age.”
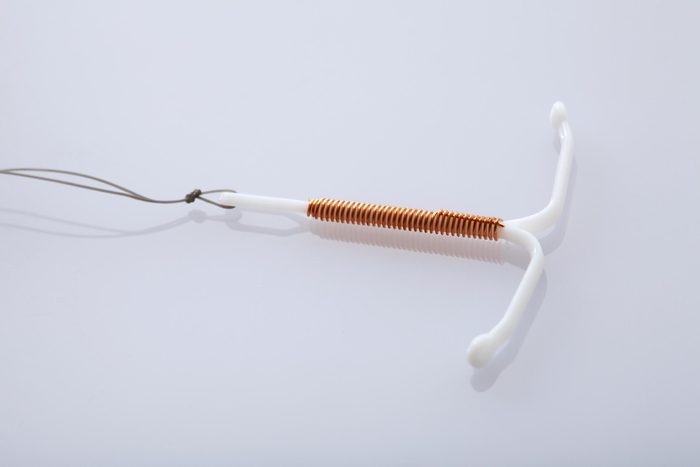
“I had a Mirena intrauterine device implanted”
Allison Martin, of Seattle, WA, was only 17 when she was diagnosed with endometriosis—something she’s grateful for, as the disease is often ignored in teen girls—most suffer an average of ten years before getting a proper diagnosis, according to the New York Times. “I was lucky to have a pushy mom who wouldn’t accept ‘some girls just have really painful periods’ as an answer,” she says. Getting diagnosed so early also gave her more options for treatment. “My doctor recommended I get a Mirena IUD and I’ve had two now—they last five years each—and they’ve worked great. I barely spot during my time of the month and have no pain now.” The Mirena IUD is a T-shaped device placed in the uterus through the cervix. It releases small amounts of synthetic progesterone and can significantly reduce bleeding and period pain for some women. Although some women worry that an IUD can hurt, that’s just one of 20 common myths gynecologists hear all the time.

“I had laparoscopic excision surgery”
“I didn’t find out I had endometriosis until I was trying to get pregnant and couldn’t,” says Jameela K., of Miami, FL. Based on her symptoms, her doctor suspected endometriosis, and he scheduled exploratory surgery using a small device called a laparoscope. “He went in and confirmed the endometriosis and then while I was still under removed all the lesions and scar tissue he could see,” she explains. That was a year ago and her symptoms are much better, though her doctor expects it to grow back eventually; at that point, she’s willing to try other surgical or medical treatments because she’s still trying to conceive. About 30 to 50 percent of women with endometriosis will suffer from infertility, according to the Endometriosis Foundation of America.
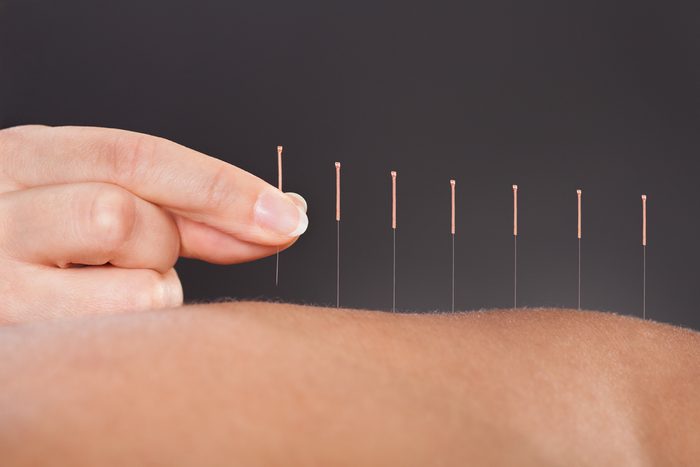
“I get acupuncture once a week”
When you’re in chronic, excruciating pain from endometriosis, you’ll try anything, no matter how weird it sounds, says Annabeth L., of British Columbia, Canada. After several ablation surgeries that helped only temporarily, Annabeth says, she finally resigned herself to just living with the disease. “I decided to focus on helping my symptoms rather than hoping for some cure,” she says. “I know it sounds woo-woo, but I’ve found real relief from the pain and cramping using acupuncture. I used to be on the floor, unable to go into work at least seven days out of every month. Now that’s down to maybe one.” She adds that she’s also switched to a vegetarian diet and does yoga three times a week, both of which also help her manage her pain and the stress from her illness. Learn about 7 more conditions where acupuncture can help.

“I eat an anti-inflammatory diet”
To get a “gold standard” diagnosis of endometriosis, women need a visual inspection by laparoscopy or, less commonly, imaging scans. There are exceptions: “My doctor discovered my endometriosis during a routine exam, he could actually see the tissue growing out over my cervix, no joke,” says Ashley Anderson, of Salt Lake City, UT. After that startling revelation, she wasn’t sure how to proceed because, unlike most patients, she didn’t have a lot of obvious symptoms. “My periods were a little heavy but probably my biggest complaint was bloating and a feeling of heaviness down there during my period,” she says. Her doctor recommended a diet to lower inflammation—especially cutting out processed foods and sugars. “It helps; I’m definitely not as bloated, and my periods have been getting more regular. I’m not as constipated as I was,” she says. That diet didn’t just help with her endo symptoms, it could extend her longevity; these 49 anti-inflammatory foods can help you live longer.

“I use electrical therapy”
Electric shocks aren’t always a bad thing—in fact, they can be quite helpful in managing chronic pain, says Portia Ross, of New York City. She had excision surgery two years ago to remove her lesions, but the doctors couldn’t get all of them, and she still has significant pain. Now she swears by a TENS (transcutaneous electrical nerve stimulation) unit for pain management. She places sticky pads on her skin wherever she has pain—usually on the abdomen and lower back—and connects them via wires to a machine that transmits a small electrical current. “Basically it provides these little shocks which overwhelm my pain sensors so my body kind of just relaxes,” she explains. “It doesn’t hurt; it feels kind of warm and prickly. But it really does help when my endo pain is awful.”

“I go for really long walks”
When you’re in crippling pain, heading outdoors for a long walk is probably the last thing you want to do—but it might be the best thing for you, says Maria A., of Boulder, CO. “I’ve had endo for over ten years and I used to practically chug ibuprofen by the bottle. A couple of years ago I got test results back that my liver was having problems, likely because of all the painkillers I was taking,” she explains. So she made a decision to go all natural. “Now when a painful flare hits, I grab my dog and go for a hike. Being outside in nature distracts me from the pain and all the exercise helps reduce cramps and soreness.” Read on to learn the 15 things no one tells you about endometriosis.
