Nose job
If you were to ask certain celebrities, they may admit to a nose job—but would say theirs were medically necessary. The truth is a bit more complicated. Rhinoplasty (a “nose job”) can be performed to correct impaired breathing caused by structural defects of the nose (such as a deviated septum, one source of chronic congestion), but it also—and often—includes aesthetic tweaks to enhance facial harmony and the proportions of the nose. Insurance covers the portion of the surgery that’s medically necessary. However, “once we’ve finished the structural work, we mark the time on the operative record,” and after that, it’s on the patient’s tab, says Deborah J. Johnson, MD, a plastic surgeon in Sacramento, CA and past president of the American Society of Plastic Surgeons (ASPS). Surgery or no surgery, these 13 health insurance tricks can save you thousands.
Otoplasty (Ear surgery)
Ear surgery, also known as otoplasty, can improve the shape, position, or proportion of the ear, according to the Mayo Clinic. It can also correct a defect from a birth defect or injury, they say. Both adults and children can benefit from otoplasty, but if you make it to adulthood without it, then any changes you might want to make “will probably be on your dime,” Dr. Johnson says. Otoplasty in adults is covered by insurance, however, when it interferes with hearing. When it isn’t covered, the average cost of otoplasty was $2,909, per 2017 statistics from the ASPS. This type of surgery isn’t as popular as the most in-demand cosmetic treatments around the country.

Eyelid Lift
When eyelids appear droopy, you might look permanently tired—but this sagging can also impair vision, according to the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS). Surgery, called blepharoplasty (eyelid lift) can correct these problems. Without insurance, the average cost is $3,026, according to the ASPS. Dr. Johnson says it actually will in two situations. The first is when extra skin weighs down the eyelid, obstructing the patient’s vision. The second is when the muscles of the upper lid become stretched out over time, leaving the patient with a sleep-eyed look that also impairs vision. This is how dermatologists and plastic surgeons look younger without an eyelid lift.

“Beauty” marks
It’s called a beauty mark, but you don’t think it’s so beautiful. If you decide to have that mole removed, will insurance cover it? According to Dr. Johnson, “even if the mole turns out to be benign, insurance will usually cover its removal if it strikes a doctor as suspicious.” Suspicious moles may include those that follow the ABCDEs the Skin Cancer Foundation lists: those that are asymmetrical, have uneven borders, are not uniform in color, moles with a diameter larger than a pencil eraser and moles that are changing, bleeding, or itching. If it does turn out to be cancerous, Dr. Johnson adds, “your insurance plan should also cover surgery to reconstruct your appearance.” Some people might confuse moles or lesions for beauty marks which is why you should check your body for these 7 skin cancer symptoms now.
Boob jobs
Breast augmentation—aka a boob job—may be covered by insurance in certain circumstances. Dr. Johnson explains that when you talk about plastic surgery covered by insurance, the question always comes down to what is “cosmetic” versus “reconstructive.” “It’s cosmetic if it’s simply the altering of the normal to make it look better but still normal. Aging is normal, so if someone comes in for work on their breasts due to the normal aging process, we consider that cosmetic,” Dr. Johnson explains. “If it’s addressing functional disabilities and deformities, it’s reconstructive.” But the notion of what is “normal” and what is a “deformity” is constantly evolving, as Johnson points out.
Since 1998, insurance companies have been required by law to cover not only breast reconstruction following mastectomy but also reconstruction of the other breast to make breasts look symmetrical and balanced after mastectomy and any physical complications at all stages of mastectomy.
This includes revising previous reconstructions, points out Maria LoTempio, MD, a New York City-based plastic surgeon specializing in reconstructive and cosmetic surgery exclusively for women. That means that following an initial reconstruction, a woman can opt for a different reconstructive approach for the purpose of enhancing the aesthetic result. Dr. LoTempio notes that the likelihood of insurance covers diminishes as time passes following the initial reconstruction, although in one case, a patient received full coverage for significant revision nearly eight years following her initial surgery. Dr. Johnson suggests that patients read their plans carefully and work closely with customer service representatives at the insurance company to determine whether the desired surgery will be covered.
Apart from breast reconstruction, breast implant revision surgery may also be covered by insurance, says the ASPS. Dr. Johnson points out that women who have already undergone a “boob job” may be able to have the removal of their implants paid for by insurance if the implants are found by a doctor to be faulty. Here’s everything you always wanted to know about breast implants.
Breast reduction
On the flipside is breast reduction surgery, a procedure where the surgeon removes fatty tissue, glandular tissue, and excess skin, says the ASPS. Beyond aesthetics, women may choose breast reduction to address physical discomfort. The ASPS says that many insurance companies cover this surgery. One downside, says Dr. Johnson, is that insurance companies tend to use cup size as a guideline (often denying coverage if you’re not a “DD or larger,” she says).
Dr. Johnson recommends documenting the symptoms and their duration. She also recommends documenting all non-surgical measures taken by the woman that have failed (such as diet, exercise, supportive bras, chiropractic, and massage). It’s also a good idea to document the woman’s willingness to endure scarring in the interest of relieving her symptoms, Dr. Johnson adds, because this shows that her desire for the surgery isn’t frivolous. (If you’re considering breast reduction surgery, here are 8 things you should know before going under the knife for breast reduction surgery, including costs, risks, and benefits.)
Male breast reduction
The American Board of Cosmetic Surgery estimates that up to 50 percent of men in the United States will experience enlarged breasts during their lifetime. For some men, the answer is gynecomastia surgery, which removes excess fat and glandular tissue for a flatter, firmer, and more masculine chest contour.
According to Dr. Johnson, insurance companies are more willing to pay for the surgery in teens and young adults than they are for older adults. There’s a common belief, she notes, that “if this guy made it through his teens and early twenties without the surgery, he’s fine,” she says. Plastic surgery before and after photos might be alluring, but before considering going under the knife read these 13 things plastic surgeons won’t tell you.
Panniculectomy
Following major weight loss, some people may be left with excess skin. Patients may choose to undergo panniculectomy, a surgical procedure to remove excess skin and fat that hangs from the belly. In terms of insurance coverage, the law is still evolving in this area, according to Dr. Johnson. “There was a time a few years back when insurers covered panniculectomy. Then they decided it was a problem of one’s own making and began to deny coverage,” she recalls. “Then the American Medical Association classified obesity as a disease, and states began requiring insurance companies to once again cover the surgery,” Dr. Johnson adds. If you’ve never heard of a panniculectomy, chances are that these unusual cosmetic surgeries will be news to you as well.
Tummy tuck
Whereas a panniculectomy removes only excess skin, a tummy tuck (also known as abdominoplasty) involves the removal of excess skin and fat from the abdomen and a tightening of the fascia that lies on the abdominal muscles, Mayo Clinic explains. A tummy tuck will be covered by insurance, however, when it is done as part of a breast reconstruction. For example, in what is known as a DIEP Flap procedure, Dr. LoTempio uses skin and fatty tissue from the abdomen to replace the skin and tissue removed from the breast during mastectomy, resulting in a soft, natural, reconstructed breast. In SIEA Flap surgery, the blood vessels in the lower abdomen, just beneath the skin, are used. Surgery isn’t necessary if you try these 23 ways to flatten your belly without surgery.
Butt lifts
The average surgeon charges $4,884 for butt implants, so wouldn’t it be nice if insurance would cover it? Spoiler: it won’t. However, if you must undergo a mastectomy for medical reasons, there are surgeons who are able to create new breasts out of skin, fat, and blood vessels removed from the gluteal area, says Dr. LoTempio. This surgery results in a newly contoured and lifted backside and is now routinely covered by insurance, she says. In fact, there are several other flap surgeries that can be performed using thigh tissue which result in a what Dr. LoTempio calls a “mini thigh lift.” Perhaps you don’t need a butt lift and the right underwear to flatter your butt shape will do.
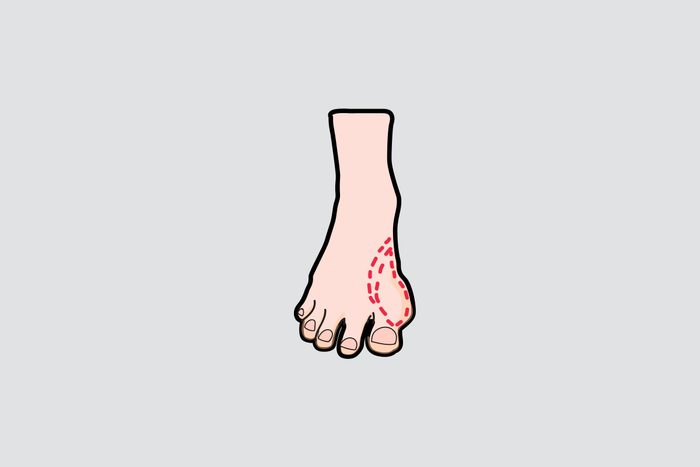
Bunions
You love those high-heeled shoes, but your feet don’t. Now you have a bunion—a painful bony bump on the joint at the inside of your toe. This is a foot deformity. According to Josef J. Geldwort, MD, DPM, a sports medicine doctor and podiatrist in New York City, “more health insurance companies will cover a bunion procedure than you may think. It all depends on the circumstances,” he says. Namely, if your bunion is causing pain and impacting your functioning. While you’re waiting for surgery, try these ways to deal with your bunion pain.
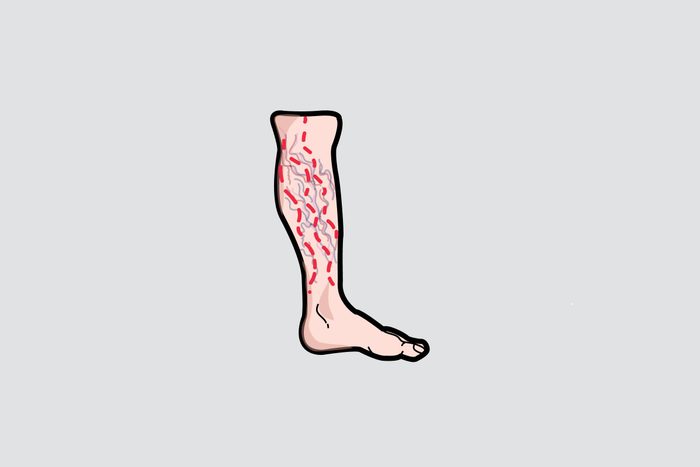
Varicose veins
“I’ve had many patients tell me that they were reluctant to see a doctor for their varicose veins because they thought varicose veins were a cosmetic problem, so their health insurance plan wouldn’t pay for treatment,” says Steven D. Cox, MD, a surgeon at Fairfield Medical Center in Lancaster, OH. It is true that most health plans will authorize treatment of varicose veins if we can demonstrate medical necessity. “If you have large, bulging veins on your legs or thighs, you probably have a problem called venous insufficiency, which meets the criteria for medical necessity for insurance plans,” he says. According to Dr. Johnson, the rule is that “generally, if your varicose veins present with painful symptoms and you’ve tried and failed with non-invasive therapies such as support stockings and sclerotherapy, then insurance will cover the surgery.” It probably won’t alleviate the need for surgery, but here’s why horse chestnuts may provide some relief for the discomfort of varicose veins.

