
The rush for research
More than 5 million Americans live with Alzheimer’s disease, a figure that’s expected to double by 2060, according to the CDC. It’s the sixth-leading cause of death in the United States.
Medical experts are hoping to change those statistics. More than 400 experimental treatments are now in U.S. clinical trials for Alzheimer’s. “We desperately need an answer,” says Heather Snyder, PhD, senior director of medical and scientific operations at the Alzheimer’s Association. “Every idea should be explored for a way to stop or slow the progression of the disease.” There are currently five FDA-approved Alzheimer’s drugs, which temporarily boost the performance of brain chemicals and slow memory decline for a short period of time. But they don’t treat the underlying decline and death of brain cells. Scientists are hopeful that one of the following areas of research may lead to a solution that will. Stop believing these 15 myths about Alzheimer’s.

New tests to catch Alzheimer’s early
At the moment, positron emission tomography imaging (PET scans) or invasive tests like sampling your cerebrospinal fluid are the only ways to catch Alzheimer’s in its early stages. But researchers have been developing blood tests that can detect amyloid beta, a toxic protein that forms the brain plaque associated with Alzheimer’s disease.
Scientists from Germany and Sweden analyzed archived blood that was collected between July 2000 and December 2002 in a study of adults ages 50 to 75. The researchers then compared the samples from adults who were later diagnosed with Alzheimer’s with those from people who didn’t develop the disease. The new test correctly identified those with Alzheimer’s in almost 70 percent of cases. Even better, this test could have spotted the disease up to eight years earlier. Another study produced a blood test that could spot Alzheimer’s even sooner—up to 20 years before diagnosis.
Even though a blood test won’t cure Alzheimer’s, it could help researchers develop treatments designed to slow the progress of the disease by identifying at-risk patients before too much damage has occurred. More work needs to be done to advance the treatment, but some researchers are hopeful that the blood test will be readily available to the public within a few years. Don’t ignore these 10 early signs of Alzheimer’s disease.
Promising new drugs
Even in the age of modern medicine, most new drugs and treatments for Alzheimer’s fail. Which is why experts are cautiously optimistic about something called BAN2401: Not only does this antibody reduce amyloid brain plaques, but it also slows cognitive decline. In the study, the New York Times reports, researchers gave 856 patients from the United States, Japan, and Europe injections of BAN2401. Doctors had previously diagnosed the patients with either mild cognitive impairment or mild Alzheimer’s dementia; they all had large amounts of amyloid beta in their brains. Only 161 patients were injected with the highest of the five doses of BAN2401—every two weeks for 18 months. In the highest-dose group, 81 percent showed significant drops in their amyloid levels. While their cognitive skills still declined, they did so at a rate that was 30 percent slower than the placebo group’s rate of decline.
More trials are needed to truly determine the drug’s effectiveness and safety before the FDA gives its stamp of approval for Alzheimer’s patients. A similar treatment, aducanumab, is in early trials and appears to do the same thing as BAN2401, but those clinical results won’t be available until 2020, according to the New York Times.

Understanding tau tangles
Tau is a protein in the brain that can twist into microscopic fibers called tangles. When this happens, cells die because nutrients can no longer move through them; the brain’s transport systems eventually disintegrate. “Tau tangles are not unique to Alzheimer’s disease,” says Snyder. “Tau clumps in other brain diseases, like Parkinson’s disease dementia, so it’s being researched in other communities as well.”
Fortunately, scientists from the University of Texas Southwestern’s O’Donnell Brain Institute have just discovered how and when a healthy tau protein becomes toxic—what the study authors call the “Big Bang” of Alzheimer’s disease. The researchers found that a tiny portion of the toxic tau protein that is normally folded inside actually sticks out, and that causes it to connect and tangle with other tau proteins. “The hunt is on to build on this finding and make a treatment that blocks the neurodegeneration process where it begins,” Marc Diamond, MD, director for UT Southwestern’s Center for Alzheimer’s and Neurodegenerative Diseases, told UT Southwestern Medical Center. Learn the differences between Alzheimer’s and dementia.

New Alzheimer’s genes
Scientists have also been looking into a possible genetic component behind Alzheimer’s disease—it does tend to run in families, after all. In one study, researchers from Boston University and the Alzheimer’s Disease Sequencing Project analyzed entire genetic sequences in nearly 6,000 people with Alzheimer’s disease, which they compared with the genes of 5,000 healthy older adults. The result? They found several rare gene variations that they believe could be linked to Alzheimer’s disease. The study authors believe that an inflammatory response in the body could trigger changes in the genes, and that could lead to brain degeneration. More research is necessary to get the whole genetic picture, but the research is promising.
Other research suggests that inheriting just one variant copy of the apolipoprotein E (APOE) gene can double your risk for Alzheimer’s disease, according to the Harvard Heart Letter. Researchers believe that the e4 variant interferes with body defenses that would block the growth of amyloid beta plaques. The only issue: Sixty percent of people who suffer from Alzheimer’s don’t have the e4 variant. “Identifying rare variants could enhance our ability to find novel therapeutic targets and advance precision medicine approaches for Alzheimer’s disease,” Eliezer Masliah, MD, director of the Division of Neuroscience at the National Institute on Aging, said in a press release. Make sure you know these 15 things no one tells you about Alzheimer’s.
Repurposing other medications
It’s possible that we already have drugs—approved to treat other conditions—that could block Alzheimer’s. One example: Yale University School of Medicine researchers found that an experimental cancer drug, saracatinib, restored memory loss and reversed brain problems in mice; they are now testing it in humans. “They are investigating a pathway that results in the activation of a protein called Fyn kinase,” says Snyder. This protein plays a major role in how clusters of beta-amyloid damage brain cells—and the cancer drug seems to block Fyn kinase. The research team recently finished collecting data on its safety, tolerability, and effectiveness in treating Alzheimer’s. A total of 159 participants received either saracatinib or a placebo for one year. The results have yet to be released.
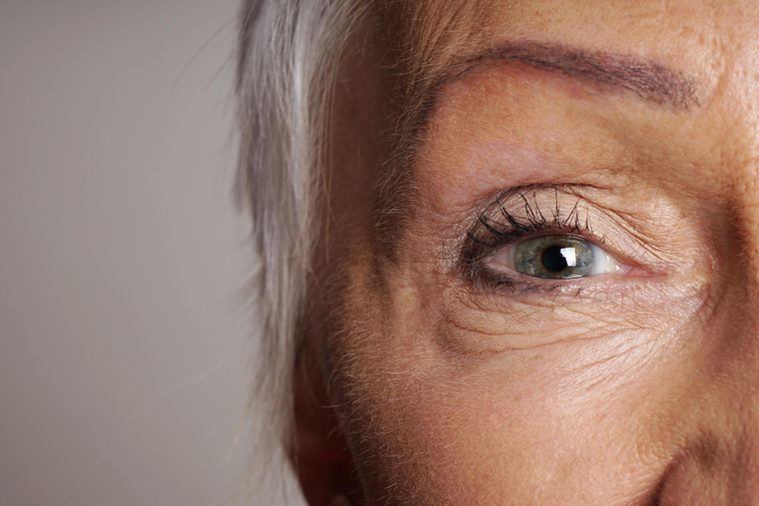
Looking outside the brain for early Alzheimer’s disease clues
Your brain may not be the only target of Alzheimer’s disease: Researchers from Cedars-Sinai Medical Center in Los Angeles used eye-imaging technology to analyze the retinas of a small group of Alzheimer’s patients. In the study, the Alzheimer’s patients had 4.7 times more amyloid beta in their eyes than the people who did not have the disease.
Another study revealed that people with rosacea (a skin condition that causes facial redness) are 7 percent more likely to develop some form of dementia and 25 percent more likely to develop Alzheimer’s disease. The inflammation of rosacea—and the proteins involved—may contribute to the development of Alzheimer’s, the study authors say. Now check out 50 everyday habits that reduce your risk of Alzheimer’s and dementia.