What is your bowel baseline?
If you exclude skin cancer, colorectal cancer is the third most common cancer in the U.S., according to the American Cancer Society. Most of the time, colorectal cancer starts as a growth or a polyp in the lining of your gastrointestinal tract. The good news is that there are a variety of tests that can pick up on these precancerous or cancerous growths, so they can be treated early. One of the most accurate tests for colorectal cancer is a colonoscopy, where a gastroenterologist examines the entire colon and rectum for abnormal growths using a lighted flexible probe.
The not-as-good news is that the prep for the test requires cleaning out the colon using laxatives or enemas. So, for example, you may need to drink a large amount of liquid laxative the day before the procedure. Everyone will tolerate colonoscopy prep differently. It depends on how your bowels are functioning before the prep.
“For instance, someone with severe irritable bowel syndrome may not tolerate a bowel prep very well,” says Jeffery Nelson, MD, the surgical director of The Center for Inflammatory Bowel and Colorectal Diseases at Mercy Medical Center, in Baltimore, Maryland. But sometimes, even people with no prior digestive problems can have issues like stomach pain or nausea. If you are constipated before prep begins, let your doctor know as he or she may suggest a laxative to help with overall prep. (These are 11 things your bowel habits can reveal about your health.)

Eat healthily before bowel prep
“It always helps to start prepping a few days prior, but it is not always feasible or desired,” says Rashmi Kumar, MD, a gastroenterologist with the Banner-University Medicine Digestive Institute in Phoenix, Arizona. If you’re able to get started a few days prior to the procedure, focus on eating low-fiber foods two to three days before the actual bowel prep. Eating foods that digest easily and leave your system quickly helps with the bowel prep. Focusing on drinking enough water before the procedure is also key. But always follow specific instructions from your gastroenterologist with respect to meals.

But stay away from these foods
A clear liquid diet is necessary the day before a colonoscopy and will be prescribed, but there are some other restrictions you should know about that begin three to seven days before. “I recommend a low-residue diet that avoids foods containing seeds, corn, nuts, and other indigestible substances,” says Dr. Kumar. Foods that are sometimes more difficult to digest and thus leave “residue” in the digestive tract make it more difficult for the gastroenterologist to see during the procedure. Anything with whole wheat in the ingredients, raw fruit or veggies with seeds or skin, legumes, beans, lentils, and popcorn, or basically any high fiber foods, should be avoided. It may seem counterintuitive, as including high-fiber foods in your diet is one of everyday habits that can help reduce your risk of colon cancer, but avoiding anything that is slow to digest will ensure the colonoscope—a thin, tube-like instrument with a light and a lens for inspecting your colon—provides a clear view for your doctor.

Mary Poppins approves this tip
The chalky taste and texture of laxative prep make the large volumes you need to drink even more difficult to swallow. But as Mary Poppins recommends, a spoonful of sugar can help the medicine go down. Dr. Kumar suggests ginger, lime, Crystal Light, or Kool-Aid powder—as long as it isn’t red or purple, which could be mistaken for blood in the colon. Gatorade and ginger ale are okay too, but if you are using a clear beverage, make sure it isn’t carbonated. Let it go flat and then mix it with the prep drink.

Get it down quick
Sweeteners alone may not be enough to get you through the nasty-tasting prep drink—many people say it’s the hardest part of a colonoscopy (even worse than the procedure itself!). Here are some more ways to make the laxative less horrible: Chill it and drink it through a straw—if you place the straw as far back on the tongue as possible, you won’t taste it as much. After you finish a dose, suck on a lemon wedge or any tart hard candy (again, no red or purple dyes) to mute the taste. Dr. Kumar suggests another familiar method: “Hold the nose and drink it as quickly as possible.”

Get past cramping and nausea
It’s not uncommon to experience bloating, abdominal cramping, or nausea while prepping. Dr. Kumar’s tip is to slow down the laxative if this happens. “The first thing to do is to take a break from drinking the bowel prep for about 30 minutes to an hour. Once the symptoms are abated or resolved, then start the bowel prep again but at a reduced rate,” advises Dr. Kumar. If nausea persists, get in touch with your doctor. “An anti-nausea medication like Zofran can be prescribed.”

Pamper your derriere
Since you’re going to be spending a lot of time on the toilet, consider scheduling your colonoscopy for a Monday morning so you can prep on Sunday. And treat yourself to some extra soft toilet paper. If you’re feeling sensitive back there, try some adult wet wipes with aloe and vitamin E in lieu of toilet paper. (Just don’t buy the wipes with alcohol—it can cause burning and irritation.) Tucks medicated wipes are helpful too; soothing products like Vaseline or Destin may also reduce chafing, says Dr. Kumar. Just don’t flush the wipes, it’s one of the bathroom mistakes you didn’t know you were making.

Don’t cheat on this
This is arguably the best colonoscopy prep tip of all: Be sure to down all the laxative drink. The amount of prep drink prescribed by your doctor is to ensure a good visualization so doctors can identify problems if they are present. “The point of the colonoscopy is to clearly see the lining of the colon to find polyps and other potentially serious problems, but the camera in the scope can’t see through solid stool, ” says Dr. Nelson. So, even if everything is coming out the other end clear before you’ve finished the laxative, continue drinking it until it’s all gone. If there’s poor visibility during the procedure, says Dr. Kumar, “you may need a repeat colonoscopy, which means a repeat clean-out process.” If you can’t tolerate drinking 2 quarts of prep liquid, ask your doctor about split-dosing. Prepopik requires you to drink just 10 ounces of prep liquid split into two doses that you drink at different intervals. After drinking the first 5 ounces, you need to drink five 8-ounce glasses of water throughout half the day; three 8-ounce glasses of water are required after the second dose.

Tell your doc if you’re taking these
If you’re taking prescription meds, NSAIDs (nonsteroidal anti-inflammatory drugs such as Motrin), or herbal supplements, give your doc the heads-up. You may have to stop or cut down prior to the procedure. “NSAIDs may increase the risk for bleeding, so it is usually advised to stop three to four days prior,” says Dr. Kumar. If you take oral meds or use insulin to manage diabetes, you’ll need to adjust the dosage prior to and on the day of the colonoscopy. Blood thinners can also pose a problem as they increase the risk of bleeding after biopsy or removal of polyps, so “hold off for a few days before,” says Dr. Kumar. “However, a patient should never hold off without discussing it with their doctor.”

Ask your doc about post bloat
After the procedure, some patients get painful bloating and gas. This is because doctors use a technique to blow gas into your colon, a process called insufflation, to get a better view. Some doctors use air while others use carbon dioxide (CO2). “Several studies have shown significantly less pain and bloating with CO2 during the procedure at one hour, at six hours, and in some studies at 24 hours, compared with air insufflation,” says Dr. Kumar. Either way, you can expect to pass gas.
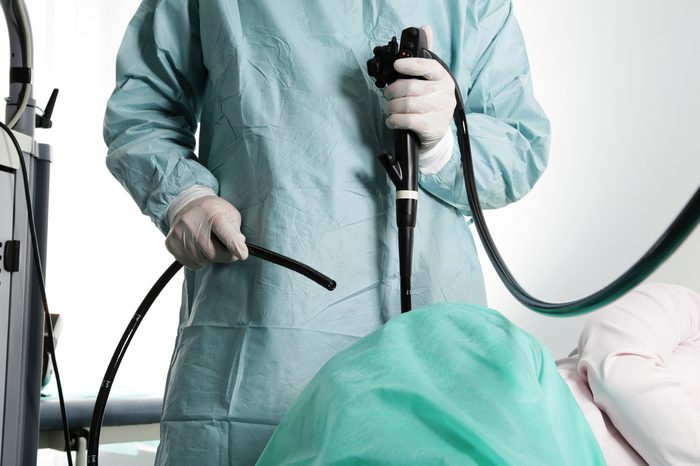
Do I really need a colonoscopy?
If you’re over the age of 45, then yes. If you’re younger, talk with your doctor about your family history to determine if you need a colonoscopy sooner. And always check in with your doctor since a variety of other symptoms including diarrhea, bloating, and bleeding could also indicate that you need a colonoscopy. You may also be able to use the at-home stool test called FIT (fecal immunochemical test) to screen for colon cancer. A review of studies published in 2019 in the Annals of Internal Medicine shows the strongest evidence to date that people at average risk for colon cancer can opt for a yearly FIT test in lieu of a colonoscopy. But what does average risk mean? “People without a family history of colon cancer in close relatives such as parents, siblings, and children, or those with no personal history of colon cancer or pre-cancerous polyps,” says gastroenterologist Douglas Corley, MD, PhD, a research scientist whose focus is colorectal cancer at Kaiser Permanente Northern California Division of Research in Oakland. A colonoscopy is the one health screening you definitely need, regardless of how healthy you are.

