6 Measles Symptoms You Should Know—Even if You Were Vaccinated
Updated: Mar. 28, 2022
The rash isn't the only symptom you need to know about.
Measles might not seem relevant, especially for people with the vaccine. But between January and April of 2019, America saw the highest reports of measles cases since the disease was “eliminated” in 2000, according to the Centers for Disease Control and Prevention (CDC). More than 700 measles cases in 22 states mean there is more curiosity and concern about measles symptoms, what the measles rash looks like, and vaccine policies. Here’s everything you need to know about the disease.
What are measles?
Measles is a highly contagious viral illness that’ll occur in 90 percent of exposed individuals, according to Bruce Polsky, MD, the Chairman of the Department of Medicine at NYU Winthrop Hospital, an infectious disease specialist. Doctors don’t over exaggerate about the measles. The virus hangs in the air for up to two hours—even after the infected person leaves the area, says John T. Raffalli, MD, FACP, a CareMount Medical Infectious Disease specialist. Here are more details on the recent measles outbreak.
What are measles symptoms?
Measles typically start with cold-like symptoms including:
- Fever
- Runny nose
- Cough
- Conjunctivitis (red eyes)
- Koplik (tiny white spots on the mouth)
- Fatigue or discomfort
These signs and symptoms appear two to four days before the rash, Dr. Polsky says, and up to three weeks after the initial exposure to the virus, per Dr. Raffalli. All of these symptoms, including the rash, work from the top of the body down. This includes a sore throat and a cough that might persist for one or two weeks after recovering from other symptoms, according to Dr. Polsky. If left untreated, more serious complications of measles include permanent brain damage, pneumonia, and middle ear damage, Dr. Raffalli adds, hence the creation of the vaccine (more on that later.)
What does the measles rash look like?
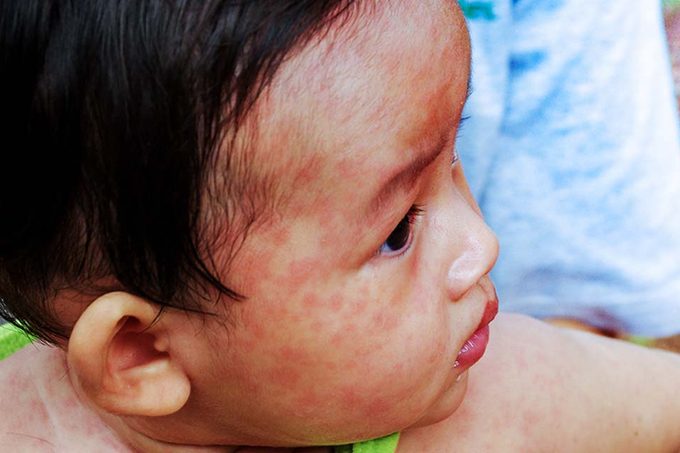
The measles rash is extremely red and blotchy. It first appears on the face, spreading downward and outward on the body to the neck, hands, and feet. If someone with measles has this rash, they are contagious via coughing and sneezing from four days before the rash appears to four days after, says Dr. Raffalli. Recognize the difference between the measles rash and 14 of the most common skin irritations.
How effective is the measles vaccine?
The global total of measles deaths decreased by 84 percent between 2000 and 2016 thanks to the measles vaccine, according to Dr. Polsky. That’s because developing the measles is rare in someone with the full vaccination—two doses of the vaccine, Dr. Polsky adds. People have the first dose between 12 and 18 months old, and the second booster between six and seven years old, Dr. Polsky says. “If you’ve only received the first dose of the vaccine, the estimated protection level is 93 percent,” he says. “We need community levels of immunity of 95 percent or greater in order to provide the ‘umbrella’ of protection that interrupts transmission.” That’s why the second shot became a staple after 1989, according to Dana Hawkinson, MD, an infectious disease specialist at The University of Kansas Health System.
Who is most at risk of measles?
The people who are most at risk for contracting the virus are those without the vaccine, such as children under one, and people who might only have one dose of the current vaccine (since doctors only began recommending the two treatments in 1989), Dr. Hawkinson says. So people with older vaccinations may need the second booster shot, which you can determine with the help of your doctor, Dr. Polsky says. People born before 1957, however, are generally considered immune as the disease was still prevalent in America during this time, before the vaccine era, according to Dr. Hawkinson. You can protect yourself against the next viral outbreak by following these 9 expert recommendations.
If you have the measles vaccine, can you still contract the virus?
There are some rare cases of contracting the virus is you have the vaccine, according to Caesar Djavaherian, an emergency medicine MD, and co-founder and Chief Medical Director at Carbon Health. “We aren’t exactly sure why, but some theories include the possibility of a subpar immune response to the vaccines to confer full immunity,” Dr. Djavaherian says. This means people with the full vaccine who still get measles might have immune systems that didn’t respond as they should have to the vaccine, per the CDC. “However, those who have been vaccinated who get measles are much more likely to have a milder illness and are less likely to spread the disease to those who are unvaccinated including young children and babies,” Dr. Djavaherian notes. In most cases, someone who has the measles vaccine shouldn’t worry, and a simple blood test can determine your immunity, Dr. Polsky adds.
So it won’t hurt for people who have both doses of the vaccine to keep an eye out for measles symptoms as both doses of the vaccine provide 97 percent—not 100 percent—protection, Dr. Polsky says. Still, Dr. Hawkinson says vaccine immunity lasts a long time. “We have a safe, effective vaccine to use to prevent measles, mumps, and rubella, two other viral illnesses,” Dr. Hawkinson says. “The most important thing you can do to keep yourself and loved ones safe is get vaccinated.” Although the vaccine is quite effective, vaccines are still one of the 11 biggest health controversies of all time.
