What is an autoimmune disease?
Your immune system is amazing, and is able to help fight off infections caused by viruses, bacteria, and a lot of other things. However, in some cases, it can unexpectedly turn on the body’s own tissues, attacking them as if they were an outside invader. This is an autoimmune disease.
“Autoimmune disease occurs when the immune system attacks a person’s own cells and tissues,” says Daniela Cihakova, MD, PhD, an immunologist at Johns Hopkins University. Autoimmune diseases include more than 80 chronic and sometimes disabling conditions, including multiple sclerosis, lupus, and type 1 diabetes, according to the National Institute of Environmental Health Sciences. This can occur in almost any part of the body, from the brain to muscles, skin, and other vital organs.
An individual’s risk for this type of disease is a combination of genetic susceptibility and some other exposure, like environmental. However, autoimmune diseases are still a mystery as they can vary in severity—from mild to life-threatening. So, should you worry about them? Read on to learn about this mysterious set of conditions and how to seek proper medical treatment.

Autoimmune diseases are increasing
The research is clear—the number of people with one of these conditions has been increasing in the last several decades. Approximately 24 million Americans are now affected, with the American Autoimmune Related Diseases Association (AARDA) putting the estimate even higher, at 50 million. “Some autoimmune disorders, such as type 1 diabetes and autoimmune thyroid disease, are thought to be on the rise,” says Emily Somers, PhD, an epidemiologist at the University of Michigan’s School of Public Health. “These changes over time suggest that environmental factors are involved.” Find out the difference between type 1 and type 2 diabetes.

They affect young women most frequently
Dr. Cihakova says about 80 percent of people with autoimmune conditions are women, with some diseases like Sjogren’s syndrome having a women-to-men ratio as high as 9:1. The U.S. Department of Health and Human Services’ Office on Women’s Health says these conditions tend to develop during the childbearing years. “Females have a higher susceptibility to autoimmune diseases than men—in fact, autoimmune diseases as a group rank among the leading 10 causes of death for women,” Dr. Somers says.
“For many years it was assumed that hormones such as estrogen were involved, but more recently, it has been suggested that genetic factors linked to the X chromosome may be involved.” Females have two X chromosomes while men only have one; the second may give an extra “dose” of X that may make women more susceptible to X-linked conditions, researchers theorize. Also, “females and males often differ in their susceptibility to the effects of environmental agents” that might impact autoimmunity, Dr. Somers says. But overall, the reason for the sex disparity is “a mystery,” she says. (Read how one woman beat chronic pain from multiple sclerosis.)

There’s a link between diseases
Doctors are ramping up studies on autoimmune conditions because since there’s limited information. “We do not yet fully understand why autoimmune diseases develop,” Dr. Cihakova says. In the past, no one came to the realization that these different types of autoimmune diseases are related. The AARDA says that much research so far has been specific to singular diseases, instead of looking at autoimmunity as a whole.
Doctors who treat autoimmune conditions tend to be in many disciplines. The Office on Women’s Health lists no fewer than seven specialties, including rheumatology, endocrinology, gastroenterology, and dermatology. Without understanding the root cause, it’s hard to sort out what’s really going on. And with vague symptoms (discussed later) from a generally healthy young population, receiving a diagnosis is not easy. (Take a look at the diseases doctors miss.)

It’s partly in your genes
Research suggests a combination of genetics and an environmental trigger may lead to the development of an autoimmune condition, Dr. Cihakova says. Interestingly, families could have a genetic susceptibility to autoimmunity in general. So, one family member may have type 1 diabetes while another has lupus, and yet another has rheumatoid arthritis. But it’s not just about genetics.
“Studies on twins show that genes alone cannot explain why certain individuals develop autoimmune diseases,” says Dr. Cihakova. “It is possible that genetically susceptible individuals develop an autoimmune disease after a certain infection, as multiple viruses have been suspected to precede autoimmune diseases.”

Environmental factors could be triggers
Environmental factors may be trigger or something outside the body could switch on the autoimmune response. “The rapid increase suggests that environmental factors play a role—a notion also supported by the fact that the increase in the incidence of autoimmune disease is evident in recent migrants to western countries,” Dr. Cihakova says.
In other words, people who move to a western country end up with the same autoimmune rates as people who were born there. Environmental risk factors range from ultraviolet radiation and asbestos to solvents in cleaning products and nail polish. “Silica dust [from working with quartz, granite and other minerals] and smoking are two risk factors for autoimmune disease,” Dr. Somers says. “Mercury is another toxicant that has been suggested to play a role in autoimmunity.” (Here’s why autoimmune diseases can feel worse during summer.)

Some lifestyle factors may protect against it
A diet rich in fruits and vegetables can be one way to ward off autoimmune conditions. “A well-balanced diet and weight control are key,” Dr. Cihakova says. “We have considerable evidence now that fat tissue is immunologically active, and that overweight and obese people have more a pro-inflammatory environment in their bodies.” Because the main symptom of autoimmunity is inflammation, weight could be a contributing factor. Dr. Cihakova also recommends exercise, which can “prevent debilitating fatigue that is often associated with an autoimmune disease.” Dr. Somers advises getting enough vitamin D and omega-3s, both of which have been shown to have a protective effect. Here are 16 foods that fight inflammation.

Lupus is difficult to diagnose
There are many autoimmune diseases, but there are a few you should know more about. One is lupus; actress Selena Gomez revealed in 2015 that she had this autoimmune condition. This disease causes inflammation in many different parts of the body, including the joints, skin, kidneys, brain, blood vessels, heart, and lungs. The Lupus Foundation of America says 16,000 new cases are reported each year in the U.S., with 1.5 million Americans living with lupus. Because lupus affects major organs, it can have life-threatening effects if not controlled with medications such as corticosteroids or immunosuppressants. Find out more silent signs of lupus you should never ignore.

Rheumatoid arthritis can affect anyone
This isn’t your grandmother’s arthritis: Rheumatoid arthritis can affect younger people and is caused by an autoimmune reaction and inflammation in the joints, not wear and tear over time, like osteoarthritis. With rheumatoid arthritis, your body attacks its own healthy joint tissue, according to the American College of Rheumatology. Symptoms include joint pain, stiffness, and swelling, most commonly in the small joints of the hands and feet. There are now better medications to treat rheumatoid arthritis than there were in the past, and they can help slow the progression of this incurable disease. Fortunately, “rheumatoid arthritis may actually be decreasing,” Dr. Somers says.
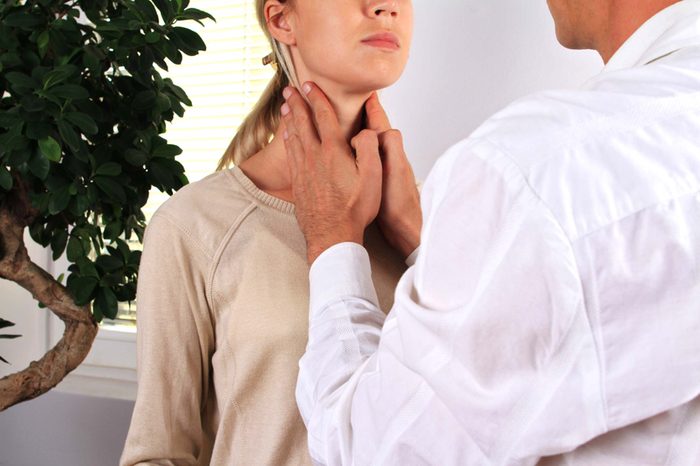
Hashimoto’s thyroiditis can be treated
In this autoimmune condition, the body attacks the thyroid gland, causing it to become underactive (hypothyroidism). According to the American Thyroid Association, as with other autoimmune-related diseases, Hashimoto’s symptoms may come on gradually and be very non-specific. They include fatigue, weight gain, constipation, sensitivity to cold, dry skin, depression, and muscle aches. You may also develop a swelling, called a goiter, in the thyroid, which is located at the front of the neck.
Luckily, a blood test for thyroid-stimulating hormone (TSH) can detect if your levels are low, and thyroid hormone replacement meds are very effective and have no side effects. Another thyroid-related autoimmune condition is Graves’ disease, which causes your thyroid to be overactive (hyperthyroid).

Celiac disease can cause lasting damage
The trigger for celiac disease is clear: When you eat gluten (found in wheat, rye, and barley) the body attacks the small intestine, causing long-term damage that could prevent the absorption of nutrients. According to the Celiac Disease Foundation, it’s also genetic, so having an immediate family member with it gives you a one in 10 chance of developing the condition yourself. Symptoms may include anemia, fatigue, bone or joint pain, depression, or skin rash. (Although you can also have no symptoms at all, even though the condition could still damage the intestines and cause other health problems.)
Treatment is a gluten-free diet, and since there are so many hidden places to find gluten (including non-foods like vitamins, lipstick, and toothpaste), it’s important to work with a dietitian to help you with the condition. Another autoimmune condition that affects the gastrointestinal tract is inflammatory bowel disease, which includes Crohn’s disease and ulcerative colitis.

Psoriasis is very visible
Although it looks like a bad skin rash, psoriasis isn’t contagious. It occurs when the body attacks its own skin cells, making too many new ones and causing a thick, red, scaly buildup. “Interestingly, men often have a worse prognosis and more severe autoimmune diseases than women,” Dr. Cihakova says.
According to the National Psoriasis Foundation, about 30 percent of people with it will also develop psoriatic arthritis, a joint inflammation, although it’s not exactly clear why. For psoriasis, treatments may include topical creams for mild cases, and a combo of creams and oral meds for more severe cases. Controlled exposure to sunlight may also help.
Other skin-related autoimmune conditions include vitiligo, in which the skin’s pigment is attacked, causing it to lose its color; and scleroderma, which causes thickening and tightening of the skin. Here are more surprising signs of disease your skin can reveal.
