Pelvic-Floor Dysfunction: Are You at Risk?
Updated: Apr. 05, 2021
An achy back, incontinence, and pelvic pain may all have one sneaky cause. And your doctor has probably never mentioned it.
The pain began like an odd muscle pull around her groin. “Within days, the area felt like it was on fire,” says Lisa, 36, a New Jersey mom of two and a human resources executive. “I’m a strong woman. But the pain was excruciating. At one point, I was curled in a ball at work, sobbing.”
It was the summer of 2012. Lisa trudged to 11 doctors in one month, but none found anything wrong. Tests for infections came back negative. Antibiotics, antivirals, and antifungals were useless. A psychiatrist hinted at marital discord (“So not true,” Lisa says). “I hated waking up and wondering if I’d get through work and be able to spend time with my kids and husband or end up just lying on the couch again,” Lisa says.
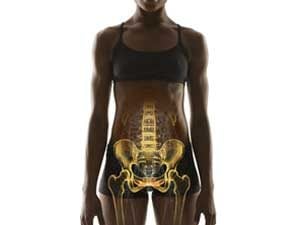
Then, as she sat in yet another doctor’s waiting room, a book caught her eye. It was Heal Pelvic Pain, by physical therapist Amy Stein. Lisa found familiar symptoms and a phrase that she’d never heard: the pelvic floor. This melon-size web of muscles, ligaments, and exquisitely sensitive nerves at the bottom of the pelvis supports the uterus, bladder, colon, and rectum. It stabilizes the trunk and hips and affects everything from orgasm to continence. If something goes awry, it can cause searing pain in a wide array of organs and tissues.
Lisa finally got her diagnosis—pelvic-floor dysfunction (PFD)—though only after she saw a pelvic-floor physical therapist. This relatively new breed of practitioner has expertise on how to fix what goes wrong in male and female pelvises.
Pelvic Pain: Who’s at Risk
For a condition so hard to diagnose, PFD is surprisingly common. By some estimates, it affects one in three American women. Giving birth boosts your chances of developing a pelvic-floor issue by 18 percent if you’ve had one child and 32 percent if you’ve had three or more, according to the Herman & Wallace Pelvic Rehabilitation Institute in Seattle.
Hormonal declines in menopause and loss of muscle mass with age are among other culprits for women. Surgery or an accident (like falling on your hip or tailbone) may play a role, as can obesity. In your 50s and 60s, your PFD risk nearly triples, compared with in your 20s or 30s.
Though pelvic-floor dysfunction is less prevalent in men, it’s still underdiagnosed. Some 90 percent of chronic prostate infections, for example, are not caused by bacteria; experts suspect a weak pelvic floor may be a factor. Surgery, injury, obesity, and chronic constipation can damage the pelvic floor in men, leading to incontinence, pain, and problems with sexual performance. Men may be embarrassed to seek treatment—and, like women, they are often misdiagnosed if they do.
For patients like Lisa, PFD manifests as pain in the vulva. In others, it presents as a bowel disorder; endometriosis; or bladder, hip, back, or abdominal pain. “Often, doctors treat symptoms in the affected organ or joint rather than find the real cause,” says Amy Stein, the pelvic-floor physical therapist in New York City whose book set Lisa on the path to a diagnosis. “They try to treat just the vulva pain, the constipation, or the hip joints. But when you miss the cause, you can’t really fix the problem.”
A Sneaky Back-Pain Trigger
Anatomically speaking, the pelvic floor is the center of your physical power, keeping both sides of your body balanced. If the muscles tighten or lose mobility, they can cause pelvic bones to torque. That’s what happened to Alexandra, a Washington, DC, lawyer in her mid-50s who struggled for years with severe back pain.
Her doctors said that her sacrum (a triangular bone at the base of the spine) and her sacroiliac joint (twin kidney-shaped bones between the sacrum and the largest pelvic bone) had rotated, twisting her spine like a wrung-out dishcloth. Conventional physical therapy, muscle relaxants, and cortisone shots had little impact.
Then she sought help from a pelvic-floor physical therapist. It turned out that scar tissue and adhesions from a hysterectomy had stiffened Alexandra’s pelvic-floor muscles, pulling her pelvic bones off center.
The Path to Real Relief
PFD is gaining recognition among pelvic-pain specialists, gastroenterologists, urologists, gynecologists, colorectal doctors, and urogynecologists, who have expertise in both bladder and pelvic health. The first step to relief is a pelvic-floor evaluation, followed by physical therapy.
“The exam is a lot like the gloved internal check a gynecologist does, although we focus on muscle function,” says Holly Tanner, a pelvic-floor physical therapist and curriculum director for the Herman & Wallace Institute. The therapist will look for tenderness, pain, and tension in the muscles. Men are diagnosed by a urologist or other specialist after a thorough examination of the groin and a rectal exam.
“This should be frontline treatment,” says urogynecologist Colleen Fitzgerald, MD, medical director of the Chronic Pelvic Pain Program at Loyola University in Chicago. “If you’re not seeing a specialist who understands the impact these muscles have on pain, you may not be getting the best care. Less than half the women who would benefit from a pelvic-floor evaluation get one.”
While there are drugs for and surgical solutions to some pelvic-floor problems, physical therapy plus home routines may help many patients feel better. A 2014 study of nearly 800 women with PFD found that most saw incontinence, constipation, and/or pain improve by at least 80 percent with pelvic-floor physical therapy. In another study, people with lower-back pain got extra relief when they added pelvic-floor exercises to back exercises and ultrasound. For Alexandra, months of pelvic-floor therapy strengthened weak muscles, easing her back pain.
Other treatments include massage-like work inside the vagina by a therapist to release tight spots, with biofeedback to train a patient to tighten and relax the muscles herself. “It’s not weird. Treatments are very professional,” says Lisa. Patients also do daily exercises at home, including Kegels to strengthen weak muscles and relaxation exercises for tense muscles, hip flexors, and glutes.
Lisa had a couple of scary pain relapses, but she got more physical therapy and continued home exercises. “My life is back to normal,” she says. “I rock-wall climb, paddleboard, and wear jeans with heels to go dancing, which I was terrified I would never do again.”