How to prevent type 2 diabetes
Although it sounds hard to believe, one in 10 adults have type 2 diabetes, and one in three have prediabetes, a condition where blood sugar is higher than normal, but not yet type 2 diabetes. That’s millions of people in the U.S. who have serious conditions that can be prevented (or at least delayed), with lifestyle changes. (Type 2 diabetes is caused by a combination of genetics and lifestyle factors, so it isn’t preventable in every case, but you can often take steps delay it.)
If you want to know how to prevent diabetes, “insulin’s action is the key,” notes Dr. Jason Fung, MD, a nephrologist and author of The Obesity Code. Dr. Fung describes how insulin, insulin resistance, and the stress hormone cortisol are the key hormonal triggers to both type 2 diabetes and obesity.
To reverse them you need to address those triggers, Dr Fung says. Here are some steps you can take that may help avoid a type 2 diabetes diagnosis.

Try intermittent fasting
Intermittent fasting involves eating only between a limited set of hours—say between 10 a.m. and 6 p.m. It may help prevent diabetes by stabilizing blood sugar, according to a study published in 2018 in Cell Metabolism. When overweight men with prediabetes ate three meals a day within a six-hour period starting around 8:30 a.m. and ending before 3 p.m, their insulin sensitivity increased, resulting in better blood-sugar control. The men’s blood pressure also improved compared with when they ate meals during a more typical 12-hour window.

Eat the rainbow
A produce-rich diet can prevent diabetes, according to a study published in 2012 in Diabetes Care from the Institute of Metabolic Science in Cambridge. After researchers studied the eating habits of more than 3,700 adults ages 40 through 79, then followed them for 11 years, they found that adults with the highest fruit and vegetable intake (about six servings daily) had a 21 percent lower risk of developing type 2 diabetes than people who ate the least (about two servings a day). Variety mattered: People who consumed 16 different kinds of produce a week were 40 percent less likely to develop diabetes than those who ate just eight different types. Have at least one fruit or veggie at every meal or snack, and change things up from day to day and week to week. (Learning to eat the rainbow changed one writer’s entire approach to food.)

Join a support group
When patients at risk for developing type 2 diabetes listened to their doctor’s advice to start a Weight Watchers’ diabetes prevention program, more than a third of them did not develop diabetes, according to a study published in 2017 in BMJ Open Diabetes Research & Care. The program included a 90-minute intro session followed by 48 weekly group meetings, and participants underwent blood tests at six and 12 months. Their average blood glucose levels improved and they lost weight. Remarkably, a third of the participants were able to get their blood sugar back to normal.

Do a gut check
The healthy bacteria in your gut produce a substance called indolepropionic acid. A high concentration of this acid in the blood may protect against type 2 diabetes, according to a study published in 2017 in Scientific Reports. Indolepropionic acid seems to promote insulin secretion by pancreatic cells, which may explain the protective effect. The study reinforces the importance of a high fiber diet, which keeps those healthy gut bacteria happy. Women should aim for 25 grams of fiber per day, while men should get 30 grams; for those over 50, shoot for 22 and 28 grams daily, respectively, according to the U.S. Department of Agriculture (USDA) Dietary Guidelines for Americans. (Here’s what will start happening to your body once you increase your fiber.)

Chill out
Stress makes everything worse—and diabetes is no exception. In fact, some studies suggest that stress may increase the risk of developing diabetes in the first place. When levels of the stress hormone cortisol are consistently high and you don’t exercise to buffer its damaging effects, you could be setting yourself up for type 2 diabetes, according to the American Diabetes Association. Many studies, including a 2017 report in Current Diabetes Reports, have found a link between stress and poor blood sugar control. When you are under stress, you are also less likely to take care of yourself and do the things you need to do to stay healthy. (Here are expert tips to shutting down stress to help prevent diabetes.)

Take a stand
In a 2012 study in Diabetes Care, researchers studied overweight and obese middle-aged adults and found that when they broke up a long bout—five hours—of sitting with two minutes of walking, their bodies had better control of post-meal blood sugar and insulin levels throughout the day compared to when they didn’t take such breaks. Researchers say that over time, preventing post-meal spikes in glucose and insulin can protect the arteries and heart from damage. Get up from your desk every 20 minutes or so. Stretch, fill up a glass of water, speak to a colleague in person, or stand up during meetings.

Strike a pose
Could downward-facing dog or a cat stretch translate to better blood-sugar numbers and a slimmer waist? Maybe. In one study in Diabetes Care, 123 people with diabetes who took yoga classes lost a few pounds and kept their glucose levels steady. In contrast, a control group who didn’t do yoga saw their levels rise. Levels of cell-damaging free radicals—which play a role in diabetes complications like vision loss and kidney damage—fell 20 percent. You don’t have to be flexible as a pool noodle to try yoga. Give a gentle online yoga video a try at home. Ready to start? Here’s a 10-minute yoga workout you can do every day at home.

Learn to love your body
People who are overweight or obese have declining insulin sensitivity—or the ability to use insulin to properly control blood sugar levels—and are therefore more likely to develop diabetes. Overweight women who took classes about body image and emotional eating lost 3.5 times more weight in a year than those who got typical diet advice in a study published in Medicine and Science in Sports and Exercise from the Technical University of Lisbon in Portugal. The biggest losers in the study dropped more than body fat: They shed worries about body shape and size and gained the emotional freedom that makes sticking with a healthy eating and activity easier. So don’t wait for the pounds to come off. Look at yourself with more compassion in the mirror, noting your most attractive features and appreciating everything that all parts of your body do for you. Here are 12 proven ways to boost your body image in 10 minutes or less.

Become label savvy
Think you’re a whiz at reading a nutrition facts panel? That’s what 33 percent of people in a study published in the Journal of the American Dietetic Association thought. But using eye-scan technology that tracked what consumers really saw, scientists found that just 9 percent consistently checked calorie counts. And only 1 percent looked at fat, sugar, and serving size on most products. Know the serving size, then check calories and fat. Make sure the carbohydrate count fits your meal plan. And look for good-for-you stuff like fiber. “Understanding the nutritional content in a food and choosing wisely is one of the most important things you can do to protect your health and prevent diabetes,” says Davida F. Kruger, a nurse and diabetes expert at Henry Ford Hospital in Detroit, and the author of The Diabetes Travel Guide. (If you’re eating out, these are the 8 menu items diabetics should always avoid.)

Rethink happy hour
Just one to two alcoholic drinks a day can significantly blur your vision if you have diabetes, report Dutch researchers. The occasional drink can fit into a healthy blood-sugar management plan and may have heart-health benefits, but it may be better to switch to “near beer” or alcohol-free wine if you like a daily drink or have worries about your eyesight. A study published in The Lancet in 2016 suggests there’s no safe level of drinking, and that any potential benefit of moderate drinking to prevent diabetes is outweighed by its risks. (Here are 9 things that happen when you stop drinking alcohol.)

Combine sneakers and dumbbells
People who got aerobic exercise (walking, riding an exercise bike, or swimming) and did strength-training exercises lost more fat and were twice as likely to see a 0.5 percent drop in their A1c (a test of long-term blood-sugar levels) than those who did just one type of exercise, according to a study published in Diabetes Care. Even if you have limited time for exercise, don’t spend it all on cardio alone. Ten to 15 minutes of strength training, two to three times a week makes a big difference. (Need tips? Here’s everything you need to know about exercising with type 2 diabetes.)

Swap white rice for brown rice
A 2012 study from researchers at Harvard University found the greater a person’s white rice intake, the higher their risk for developing type 2 diabetes. The researchers examined the data from more than 350,000 participants over the course of four to 22 years. Compared with its brown counterpart, white rice has lower levels of fiber, magnesium, and vitamins. In addition, white rice is considered a high glycemic food, which means it’s digested quickly and can lead to blood sugar spikes. If you hate the taste of brown rice, try mixing it with white to help your taste buds adjust, gradually upping the proportion of brown to white. Or consider one of these good carbs for diabetics.

Keep an eye on dairy
When it comes to dairy, the jury is still out, explains Dr. Fung. There are studies, like one in Diabetes Care, that show dairy intake associated with increased diabetes risk while others show dairy intake associated with a modestly lower incidence. There’s no question dairy raises insulin, he says. “Since fat and protein do not raise blood sugar, there should be no effect on insulin. But proteins and their constituent parts—the amino acids can also raise insulin without any effect on the blood sugar,” he writes on his blog. (Here are 6 dairy myths you need to stop believing.)

Build a support team
Teaming up with family members, the doctor, and the doctor’s staff helped people with diabetes increase their success at hitting healthy blood sugar, cholesterol, and blood pressure numbers; they were a whopping 40 percent more likely to compared to those who went solo, finds a recent University of Pittsburgh study published in Diabetes Care. Assemble your own support team. Ask family members for emotional support and ask your doctor and other diabetes professionals, such as a certified diabetes educator or registered dietitian, for guidance.

Limit caffeine
While some evidence suggests coffee may lower diabetes risk, the beverage may be trickier for people who already have the disease. Research from Duke University found that people who took a sugar pill plus a cup of joe’s worth of caffeine saw blood sugar rise 21 percent higher than those who just got the sugar. Also: Insulin, the hormone that helps your body turn sugar (glucose) into energy, rose 48 percent higher in people who got caffeine. That’s bad news because it could be a sign that caffeine leads to insulin resistance, a condition in which cells have trouble absorbing blood sugar. If your post-meal blood sugar levels are higher than you like, the culprit might not be what you’re eating—it could be the caffeine in your cup. Try decaf, herbal tea, or water instead of coffee or other caffeinated drinks.

Snag more shut-eye
A bad night’s sleep can raise morning blood sugar 23 percent and insulin resistance by 82 percent, finds a large study from the University of Chicago published in Sleep Medicine Clinics. The researches say trouble falling asleep, trouble staying asleep, and sleep apnea worsened blood-sugar control in study volunteers with diabetes. A 2018 study in Endocrinology and Metabolism found that losing a single night’s sleep may interfere with the liver’s ability to produce glucose and process insulin, increasing the risk of type 2 diabetes. If you’re not waking up refreshed, take action. Banish coffee and caffeine after noon, try to exercise earlier in the day rather than close to bedtime, and keep your boudoir dark and cool at night. Take signs of sleep apnea—disordered breathing during slumber like snorting, gasping, loud snoring, and breathing pauses during sleep—seriously: See your doctor for an evaluation. (Here are nine myths about sleep you need to stop believing.)

Hoop it up
University of Wisconsin research shows that hula-hooping burns 210 calories in just 30 minutes and raises your heart rate as much as a brisk walk. Translation: This retro toy is actually a great piece of exercise equipment that can improve your cardiovascular fitness, burn calories, and improve blood sugar control. You can hula-hoop indoors or out, and it’s so much fun you won’t even think it’s exercise. Hooping has always been popular with the grammar-school set, but in recent years, adults have turned it into a hot fitness trend. It’s easy to find all sorts of hoops and hoop-related exercise information online. Of course, you can always find a classic version at a toy store too. Learn more about making weighted hula hoops part of your exercise regimen.

Relish the magic of salad
Fiber, magnesium, and polyphenols in these leafy greens can help your cells maintain their sensitivity to insulin, the hormone responsible for blood-sugar absorption, finds a British Medical Journal study. Have a salad of leafy greens every day.

Eat more healthy fats
Switching from the standard American diet to one higher in natural fats and lower in refined carbohydrates like bread and pasta can help anyone battling obesity or diabetes, says Dr. Fung. “Simply put, dietary fat does not raise insulin,” writes Dr. Fung at Intensive Dietary Management. “Hyperinsulinemia is the main driver of obesity. Hyperinsulinemia means literally, high insulin in the blood… So, logically, switching refined carbohydrates (which raises insulin) for dietary fat can lower insulin levels significantly, even if you take in the same total number of calories.”
Dr. Fung recommends the keto diet to his diabetes patients. Here’s what doctors want you to know about the keto diet.

Don’t let aches immobilize you
Half of all people with diabetes also have arthritis. Getting vital physical activity can be tough when your joints ache, swell, or don’t want to bend. That’s dangerous—and common: Half of all women and 40 percent of all men with arthritis qualify as couch potatoes, according to a Northwestern University study. Just one in nine got the 150 minutes of activity per week recommended for good health. Moving when your knees, hips, back, shoulders, or ankles hurt isn’t easy, but don’t give up. Talk to your doctor about pain medications and other treatments. Check out these everyday habits that can reduce your risk of arthritis.

Protect your emotional health
Depression and diabetes commonly occur together, but treating them simultaneously can mean a better recovery on both fronts, according to research published in Annals of Family Medicine. Researchers studied 180 patients with depression and type 2 diabetes who received treatment for both and took part in a program on adhering to medication regimens. After 12 weeks, 61 percent of patients had better blood sugar tests, and nearly the same number had fewer depression symptoms.
If you’re experiencing depression symptoms (such as sleeping more or less than usual, a lack of interest in things and activities you usually love, a change in eating habits) talk to your doctor about getting the right treatment. (Here are 8 hidden signs of depression to look out for.)

Have protein at breakfast
A 2014 study in Obesity shows that eating a large high protein breakfast is better at controlling blood sugar than eating a smaller high carb breakfast. Everyone’s blood sugar tends to be elevated first thing in the morning. A high protein/low carb meal evokes less insulin response, allowing blood sugar levels to come down. Conversely, eating a high carb meal when blood sugar is already elevated means blood sugars remain high throughout the day. (Learn more of the best and worst foods to help prevent diabetes.)

Protect yourself from plastics
High blood levels of common chemicals called phthalates are associated with about double the risk of type 2 diabetes, according to a Swedish study of more than 1,000 older men and women published in Diabetes Care. They’re found in such wide-ranging products as building materials, clothing, cosmetics, and personal-care products, food packaging, toys, perfumes, and vinyl products. While the study can’t prove that phthalate exposure causes diabetes, researchers suspect the chemicals may raise your risk by disrupting insulin production. Because phthalates are found in so many products, it’s hard to avoid them entirely—but you can reduce your exposure: Avoid plastic containers with the recycling symbol #3 on the bottom (it designates products that contain PVC, a type of plastic that has the additives). Buy phthalate-free beauty products and skip those that contain “fragrance” as an ingredient. Ventilate your home: Indoor air tends to have higher phthalate levels than outdoor air. Don’t miss these 10 other life-saving things you must do if you have diabetes.”

Grab a buddy
It’s easy to blow off an exercise plan—unless you’re meeting a friend. “You are more likely to stick with it if you are meeting a buddy,” says Kruger. Plan to walk with a co-worker during your lunch break, for example, or make an after-work workout plan with a friend. Don’t miss these 17 gym hacks that make working out less of a chore.

Take a break
All work and no play may increase your risk for diabetes. Women—but not men—who clock 45 or more hours a week have at least a 50 percent increased risk of developing type 2 diabetes, compared to women who log 35 to 40 hours weekly, finds a study in BMJ Diabetes Research and Care. The study authors speculate that working such long hours may trigger a stress response that leads to hormone imbalances, insulin resistance, and contributes to the development of diabetes. If you must work extra hours to make ends meet, be sure to exercise, eat healthy, and practice stress relief to lower your risk for diabetes.

Walk to work
People who walk to work are 40 percent less likely to have diabetes than those who drive, according to a study published in the American Journal of Preventive Medicine. People who walk to work were also 17 percent less likely than those who drive to have high blood pressure; cyclists were half as likely to have diabetes as drivers. Scheduling walking meetings is another way to get in shape without working out.

Watch your vitamin D
Researchers have linked depleted blood levels of vitamin D to a host of diseases and conditions, including type 2 diabetes. In a study published in 2018 in PLOS One, participants with higher D levels had a lower risk for developing diabetes. The precise mechanism is unclear, but one theory is that insulin-producing cells in the pancreas need vitamin D to stimulate the insulin production. More research is needed to study the possible connection. Are you getting enough? Check out these 9 signs that you may be falling short on vitamin D.

Do a shot
Of apple cider vinegar, that is. Apple cider vinegar helps keep blood sugar levels in check and will keep you feeling fuller longer. Learn more about all of the ways that apple cider vinegar could benefit your health.

Get moving
Even a short stint on the couch can up type 2 diabetes risk in at-risk seniors. In one 2017 study in the Journals of Gerontology, overweight seniors with prediabetes were asked to reduce their daily steps to no more than 1,000 a day for two weeks. Their blood sugar dramatically rose, speeding the onset of type 2 diabetes. “If people are going to be off their feet for an extended period they need to work actively to recover their ability to handle blood sugar,” said study author Stuart Phillips, PhD, a professor in the Department of Kinesiology at McMaster University in Hamilton, Ontario, Canada, in a news release. Not sure how active you are? Consider an old-school pedometer. Here are 10 reasons you’re better off with a pedometer than a fitness tracker.

Sip some green tea
When 120 overweight women at risk for diabetes consumed green tea extract (1 gram), the diabetes drug Metformin, or green tea with Metformin, those who took green tea extract showed better blood sugar control than the Metformin groups. The study appears in Clinical Nutrition ESPEN. Here are 8 health benefits of green tea you haven’t heard of before.

Get a healthy start
Due to the epidemic of childhood obesity, diseases doctors only used to see in adulthood—such as type 2 diabetes—they’re now diagnosing in kids. Research shows that when overweight children slim down before puberty, their risk of type 2 diabetes decreases dramatically. Later weight loss also lowers the risk of type 2 diabetes in adulthood—just not as much, according to a 2018 study in the New England Journal of Medicine. Addressing weight with your child is a sensitive matter. Here’s how to talk to your kids about weight.

Kick the habit
Add diabetes to the list of diseases that smoking can cause or make worse. The more cigarettes you smoke, the higher your risk for type 2 diabetes. What’s more, if you have diabetes, smoking makes it harder to control and increases your chances of developing serious health problems related to your diabetes, says the American Diabetes Association. Here are the 23 best ways to quit smoking for good.
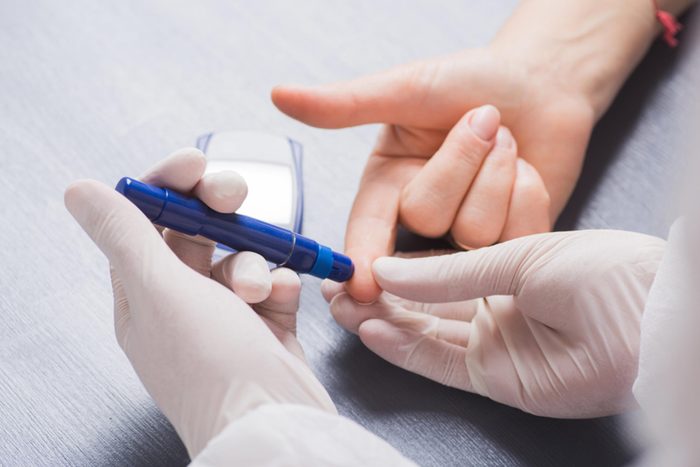
Know your numbers
In its earliest stages, type 2 diabetes can be insidious. The best way to stay a step ahead is to know and monitor your blood cholesterol, blood pressure, blood sugar, and weight. Your doctor can help you make sure your numbers are in the “safe” range and give you advice on how to lower them if they are too high. Knowing your numbers is one of the 26 anti-aging secrets that can add years to your life.

Get serious
You can lower your risk for type 2 diabetes by 58 percent if you lose 7 percent of your body weight and exercise moderately 30 minutes a day five days a week, according to the American Diabetes Association.

Go nuts
Eating almonds as part of a healthy diet can help keep blood sugar levels in the normal range and lower other risks for heart disease in people with type 2 diabetes, finds a study in Metabolism. There are roughly 23 almonds in an ounce; participants ate 2 ounces a day by incorporating roasted, unsalted whole almonds into entrees, desserts, or snacks, replacing 20 percent of the calories in their diet.

Deep six the soda
In the Nurses’ Health Study II, women who drank one or more sugar-sweetened beverages a day were 83 percent more likely to develop diabetes, compared to women who drank less than one sugar-sweetened beverage per month. “Replace soda with water or sparkling water,” says Boston-based nutritionist Dana Greene, MS, RD, LDN. “Diet soda is no better and has also been linked to diabetes risk,” she warns. Here are 12 things that will happen to your body if you give up diet soda.

Know that all red meats are not equal
Older studies that investigated a link between red meat consumption and diabetes risk failed to distinguish processed red meat from unprocessed. A 2010 study from the Harvard School of Public Health published in Circulation looked at both and found that whereas eating processed meat—such as bacon, sausage, or deli slices—was associated with a 19% higher risk of type 2 diabetes, eating unprocessed red meat, such as beef, pork, or lamb, was not associated with diabetes risk. Meat is rich in protein, minerals such as iron and zinc, and B vitamins. Those who don’t eat meat fall short on B vitamins, especially B12, which you can only get from meat, eggs, and poultry. (Here are the silent signs you may not be getting enough vitamin B12.)

Just say no to bacon
One study in the American Journal of Clinical Nutrition found that eating even small amounts of processed red meat each day (think one hot dog or sausage or two slices of bacon) increased diabetes risk by 51 percent. “Choose lean proteins such as fish and chicken instead of red and processed meats,” says Greene. Processed meats are high on the list of foods that cancer doctors try to avoid.
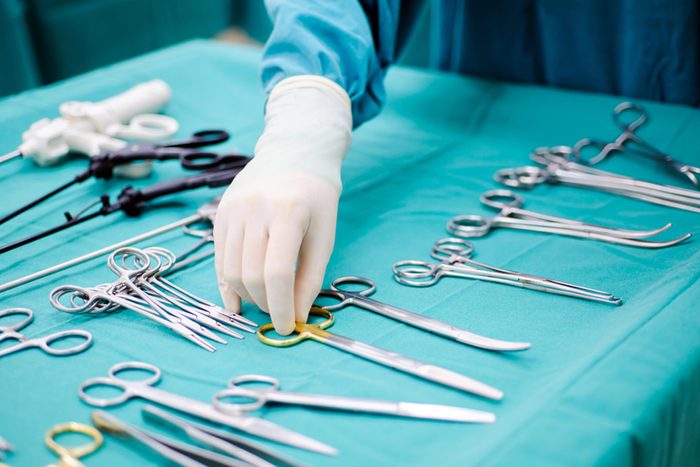
Consider weight loss surgery
Losing weight and keeping it off isn’t easy. If you are obese and already have high blood sugar or other conditions related to your weight, bariatric surgery may do more than just reduce your diabetes risk—it may save your life. According to a joint statement endorsed by 45 international professional organizations, weight-loss surgery should be considered a treatment option for people with diabetes who are mildly obese and fail to respond to conventional treatment. The Statement and Clinical Guidelines appear in Diabetes Care. (Get the scoop on the types of weight loss surgeries here.)

Get personal
Guidelines from the American Diabetes Association and the European Association for the Study of Diabetes say blood sugar goals should be based on individual risk factors, such as age, health status, and diabetes complications. Doctors may recommend hitting a lower A1c level in people who are younger and have no risk factors for heart disease or serious bouts with low blood sugar. People 65 and older with some of these issues may have less rigid numbers to hit, in part because of concerns about low blood sugar levels and side effects from too many medications. The guidelines also recommend metformin as a first-line type 2 diabetes treatment (unless a patient has near-normal A1C numbers and is highly motivated to make lifestyle changes). Other drugs can be added if after three months blood sugar levels aren’t controlled on metformin alone.

