
Nurses know best
In the age of colds, flus, and COVID-19, it’s more important than ever to keep ourselves as healthy as possible. As much as you mask, sanitize, and social distance, you might still be participating in unhygienic habits you weren’t even aware of. These are the mistakes nurses frequently see people making, from wearing your mask improperly to touching your face while you’re grocery shopping.
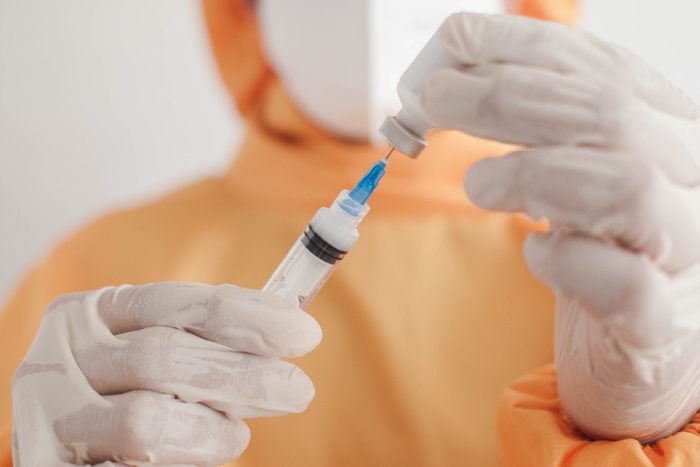
Skipping vaccinations
We might not all have the opportunity to get the COVID vaccine yet—but we can still do our part to keep our immune systems in good shape. Staying up to date on vaccines is important for adults, not just kids, says pediatric nurse practitioner Patsy Stinchfield, RN, vice president of the National Foundation for Infectious Diseases. “Adults are an important part of the community immunity we all need—when adults protect themselves against vaccine-preventable diseases, they also protect others [by not getting sick and spreading the disease further],” explains Stinchfield. What’s more, “being current on vaccines can prevent an adult from getting very ill, missing school or work, and having unnecessary expenses related to being sick. Even healthy young adults can be struck with a life-ending disease such as influenza. Prevention is better than treatment.” As we age, the immunity gained from certain childhood vaccinations wanes, so she recommends that you review the recommended adult vaccination schedule from the U.S. Centers for Disease Control and Prevention (CDC), and check your vaccination history at your next doctor appointment.

Pulling your mask down when you talk
Muffled conversations are an irritating fact of COVID-life. So it’s no surprise that several nurses we talked to said they see far too many people tugging down their masks in order to make themselves heard. But speaking sends droplets—that could be loaded with virus—into the air toward your conversation partner. You can’t be sure that you’re not infected, since many cases are asymptomatic. Ane even if you’re in the clear, “pushing the mask down below the chin could spread virus from the outside of your mask to the inside, or to the face and neck,” where they could infect you, says Karin Russ, MS, RN, clinical instructor at University of Maryland School of Nursing.
That’s why it’s key to keep your mask on when you’re talking, even when it’s inconvenient. “If others are having a hard time hearing you, speak slower and enunciate,” says Lauren Bryan, RN, MPH, CCRN-K, CPH, CIC, an infection preventionist at UCHealth Yampa Valley Medical Center, in Steamboat Springs, Colorado.

Wearing your mask below your nose
This is a mistake Angela Campos, RN, a registered nurse who specializes in critical care in Cumberland Foreside, Maine, says she sees “every single day.” Droplets that could be carrying COVID-19 come out of a person’s mouth and your nose, per the World Health Organization (WHO). So if you’re not covering your nose, it reduces the effectiveness of wearing a mask.

Re-wearing a disposable mask
According to the U.S. Centers for Disease Control and Prevention (CDC), disposable masks should be discarded after every use. But, if you absolutely need to re-wear one, Bryan says you can, with a big caveat. “Remember—the outside of the mask has filtered the contaminates that you didn’t want to inhale,” she says. That’s why it’s important not to flip the mask when you re-wear it—the side previously on the outside needs to stay on the outside. Store the mask in a paper bag to dry and prevent it from cross-contaminating other surfaces. If you do re-wear, remember to wash your hands after handling.
“The most important thing is that the mask remains dry,” Russ says. “If you are wearing a paper mask for a very short period of time, and it remains dry, the mask could probably be hung up and used again for another short period of time.” If that’s not the case, or if you cannot complete all the steps above, it’s time to throw the mask away.

Expanding your pod too quickly
As vaccines roll out across the United States, it may be tempting to resume your normal social life and start seeing more people. But take care, says Bryan. While the COVID-19 vaccines slash a recipient’s risk of severe illness or death from the virus, they don’t necessarily protect the vaccinated person from “catching” it. And a vaccinated person may be able to contract coronavirus and unknowingly spread it to others while feeling fine and experiencing no symptoms themselves.
“We still need to wait to have larger ‘pods’ until everyone in that pod has been vaccinated,” she says. “For instance, I have been vaccinated, but I can’t interact socially with my vaccinated friends yet because I could acquire an asymptomatic case and transmit it to my husband who is unvaccinated.” Check out these 13 true stories that show what happens when you don’t social-distance and expand your bubble too soon.

Not washing your hands after touching high-traffic surfaces
“I constantly see people touch their face after touching doorknobs and hand railings,” says Jeremy Hulsker, RN, CEN, Emergency Department Charge Nurse at UCHealth Memorial Hospital in Colorado Springs, Colorado. He also notes many patients forget to wash their hands after they blow their noses. If you’re away from home and there isn’t a bathroom in sight, there are still safe ways to disinfect. “A substitute for handwashing can be hand sanitizer that is made of at least 60 percent alcohol,” Campos says. “Make sure that your hands are completely covered, including in between the fingers and around nail beds.” These are the 12 dirtiest surfaces you encounter all the time.

Wearing ineffective face coverings
There’s a common misconception that things like bandanas and knit gaiters are equal to masks in preventing infection, Russ says. However, such thinly woven materials don’t offer enough protection against COVID. “Better choices in cloth face coverings would include tightly woven two- or three-layer fabric masks that fit snugly over the nose chin and at the sides of the face,” Russ says. “A cotton or polypropylene filter may add an extra layer of protection in a cloth mask. KN95 and the new KF94 mask from Korea are even better choices than cloth masks.”

Nibbling on your nails
Most people consider nail-biting a bad habit, but there are also serious health risks associated with it, says Angela Campos, RN, a registered nurse who specializes in critical care in Cumberland Foreside, Maine. “Fingernails are an ideal breeding ground for bacteria like E.coli and salmonella that are transmitted by food. When people chew their nails, this bacteria can quickly enter mucous membranes in the mouth leading to illness.” The consequences of getting sick are elevated during the COVID pandemic, especially if you put your hands in your mouth before you’ve washed them thoroughly.

Wearing your shoes in the house
“Our shoes act as a vector, picking up allergens—dirt, dust, mold spores, chemicals, bacteria, and viruses—wherever we go,” warns Lauren Bryan, RN, MPH, an infection preventionist at UCHealth Yampa Valley Medical Center in Steamboat Springs, Colorado. “You can imagine the scenario for cross-contamination: shoes with the stomach bug norovirus on them from the grocery store come home and contaminate the floor where you set your handbag, your child then lifts the purse to get a piece of gum out of the bag, then with bacteria on their hands they put the gum into their mouth. Norovirus can live for weeks on a surface and it only takes a few viral particles to make you sick.”
So instead of bringing all of that stuff into and around your house, Bryan advises leaving your shoes in the mudroom, garage, porch, or a bin in the entryway. “Just don’t set a shoe rack indoors next to an air vent or it will aerosolize all of those particulates on your shoes.” And remember to wash your hands or use hand sanitizer after tying your laces or otherwise handling your shoes, she says. While you’re at it, here are 4 household products that kill coronavirus.

Sleeping on dirty sheets
“Even if they’re not stinky or visibly soiled, sheets need to be changed weekly,” says infectious disease specialist Natalie Ingmire, MSN, RN, director of quality and patient safety at Centura Health at Avista Adventist Hospital in Louisville, Colorado. Why? Dust mites. The mites themselves aren’t harmful to humans, notes Ingmire, but their droppings are known to trigger respiratory problems, especially in those with allergies to the mites. Learn more about why you really need to wash your sheets every week.

Never wiping down your purse or wallet
How many times have you wiped down your wallet or purse? If you’re like most people, probably never until COVID-19 struck. “You may not think to sanitize your purse, but you should,” says Ingmire. “All those important things that you keep in it—phone, keys, credit cards—come in daily contact with the world and can harbor all kinds of nastiness. A nurse will wipe down wallets, purses, and keys with a Clorox wipe once in a while.”

Ignoring the TV remote on cleaning day
“Even if you’re a good hand-washer, hands are rarely 100 percent clean at home, and the TV remote catches all those germs,” says Ingmire. “So wipe the remote down with a disinfecting wipe, especially on vacation when you have no clue as to the last time your hotel remote was sanitized.”

Borrowing a swipe of lip balm
“Sharing makeup or Chapstick is the quickest way to spread cold sores and other infections,” says Ingmire. “If I have an eye infection and you use my mascara, you’re getting it. And, if I keep using my own infected makeup, I’ll keep infecting myself!” So it’s important not to share makeup, and to throw yours away and replace it after an infection.

Using kitchen sponges for too long
“Sponges are the heavy lifter in the house in terms of clean up, but if you don’t replace them frequently, you’ll spread nasty stuff like salmonella everywhere,” warns Ingmire. Several studies have found high levels of bacteria in used kitchen sponges, including one published in 2017 in the journal Scientific Reports, that found several germs that can cause illness in people, including fecal bacteria (when this shows up in the kitchen, it’s usually from meats, not your own bathroom).
“I don’t own one and never will,” says Ingmire. But if you like using sponges to wash dishes and counters, be sure to disinfect them regularly. The Good Housekeeping Institute and EMSL Analytical testing lab tested several different methods and found that the number one way to kill bacteria in your kitchen sponge is to soak it for five minutes in a mixture of 3/4 cup of bleach in one gallon of water, then rinse. The second-best method: Soak with water and microwave for one to two minutes.
Keeping secrets from your medical provider
“We all know what we should be doing—limiting gatherings, staying masked—but it’s hard, and we all have COVID fatigue,” Bryan says. But being dishonest with your doctor when you think you may have COVID makes contact tracing much more difficult, exposes others unnecessarily, and changes the follow-up procedures the doctor will give you. For example, depending on the length of time since your exposure, your doctor may want to test you for antibodies, rather than the virus itself, Bryan says.
Being open and honest with your healthcare providers is incredibly important, but too many people let embarrassment or worry get in their way, says Melissa Rubio, PhD, APRN, a nurse practitioner at the Lung Health Institute. “Sometimes patients will answer what they think their provider wants to hear, rather than what is real,” says Rubio. You may say you don’t smoke or drink, for example, when you might do so occasionally in a social setting. Or you may say you eat healthier or get more exercise than you really do. “When that happens, providers lose the opportunity to educate patients about a healthy lifestyle, especially if we already think you have a good handle on your health. Trust me, all of us can learn a thing or two about healthier living, and we also realize that our patients are human, and no one is perfect all the time.”
If you find yourself staying mum and not being truthful because you don’t feel comfortable with your particular doctor or have had a bad experience with him or her, “it is perfectly OK to search for a provider who makes you feel comfortable, matches your energy and meets your needs,” says Rubio. “We are not offended if you feel that we are not a good match.”

Not having a regular bedtime
“The current lack of respect for sleep in our society that suggests you’ll be able to catch up on sleep later is dead wrong. You can never fully catch up on missed sleep,” says Valerie E. Rogers, PhD, RN, CPNP, assistant professor, University of Maryland School of Nursing. “The chronic sleep deprivation we subject ourselves to on a daily basis has important consequences for health including weight gain, lowered ability to fight off infections, and poorer heart and digestive health.” Not only that, but lack of sleep can also take a serious toll on mental health and fuel depression and/or anxiety, says Campos. Most adults need between seven and nine hours of sleep, according to the National Sleep Foundation.

Getting too much light at night
“We are healthiest when we maintain our body’s alignment with the Earth’s day and night cycle,” says Rogers. Light from electronic devices and television can delay hormonal processes that help you get sleepy at night, leading to chronic sleep deprivation. “In the evening and at night, dim room lights and use programs on your electronic devices such as cell phones, tablets, and computers that dim the level of light emitted from screens.” Or, even better, just shut them off an hour before you intend to go to sleep.

Relying on alcohol to relax you
Don’t use alcohol as a sleeping aid, says Rogers. “The seduction of using alcohol to help you sleep is that it makes you feel sleepy and fall asleep easier. But as your blood alcohol level drops during the night, your sleep is repeatedly disturbed, and you’ll probably find you don’t feel well-rested in the morning.” Another reason you may feel groggy in the morning is that alcohol blocks REM sleep, the most restorative kind, according to the National Sleep Foundation. What’s more, alcohol relaxes muscles in your throat which increases snoring and can make sleep apnea worse.

Rubbing your eyes
“I always preach to never rub your eyes—or pick your nose—with dirty hands,” says registered nurse Jackie Dardis, RN, BSN, a heart rhythm coordinator at UCHealth. Cold viruses enter the body through mucous membranes such as those in the nose and eyes, so you could be introducing infectious viruses that you’ve touched during the day directly into your body without knowing it. “You can sit next to somebody all day long that has a cold and not catch it if you never touch your face with unwashed hands.”

Driving drowsy
Driving while sleep deprived is incredibly dangerous, says Terry Cralle, RN, clinical sleep educator and Saatva sleep consultant. “I don’t even like the term drowsy driving because it does not sound as serious as it really is. According to the CDC, drowsy drivers have slower reaction times, pay less attention to the road, and make poor decisions while driving.” Even worse, sleep deprivation impairs our clear thinking and insight. “So even when our performance plummets as a result of sleep deprivation, we will think we are performing just fine,” says Cralle. “Unfortunately, we are all busy and too often, the thing we skimp on is sleep.” Try one of these popular sleep products on Amazon that can help you catch some ZZZs.

Blasting music in your headphones
Listening to too-loud music through your headphones can impair your hearing in two ways: high volume and prolonged duration, explains Ashley Wood, RN, BSN, a contributor at Demystifying Your Health. “It’s important to follow the basic rule that the louder the volume, the shorter the duration that you listen should be. In general, you should listen to music for no more than 60 minutes a day at 60 percent of the device’s maximum volume—this is known as the 60/60 rule. If you listen at max volume, it should only be for about five minutes a day. Both Android and iOS have apps that you can use to set volume controls. This is especially useful for parents who are concerned about their kids listening to music too loudly.”
If you use your headphones often in noisy places like city sidewalks, invest in a good pair of noise-canceling headphones, suggests Wood. “These are great because by reducing the amount of ambient noise, they allow you to listen to music at a lower volume than you would if you were using regular headphones. Your hearing is incredibly important and once the damage is done, it can’t be undone.”

Brushing, but not flossing
Flossing isn’t just about the health of your teeth, says Wood. “The plaque that builds up on your teeth also builds ups under your gum line and between your teeth. When there’s too much of it, you can end up with gum disease. This might not seem horrible, but it’s linked to other health issues, such as stroke, heart disease, and diabetes.”

Going overboard on booze
It can be easy to drink too much when you’ve been in quarantine for so long, or are finally attending a Zoom happy hour with friends. It can be easy to drink too much when you’re with friends you haven’t seen for a while, or at a party where the host keeps filling your glass, says Teri Dreher, RN, owner and CEO of NShore Patient Advocates. But even one drinking binge causes an elevation in liver enzymes, she says. And if this behavior becomes more frequent or you start doing it when having strong negative emotions, there is an even greater risk: “Depression is made worse by alcohol. [And] as people get older, especially if they are alone, they may drift into alcoholism surprisingly easily. If you are in doubt about your drinking tendency, take the ’30 day challenge’ [where you abstain from alcohol for 30 days] and if you cannot abstain and need help, find a local AA meeting or rehab right away. Alcoholism does not only cause physical damage but heartbreaking family stress that can be remedied if caught in time. It is never too late to quit drinking.” Use these 17 tips to help you cut back on drinking.

Letting people hold your newborn
As tempting as it may be to let friends and family members in your pod hold your baby, it’s better to be safe than sorry. “As a neonatal nurse practitioner who has cared for thousands of critically sick babies, this is one major thing I’d love to see new parents stop doing that puts their newborns at risk,” says Traci Powell, MSN, APRN, a neonatal nurse practitioner at Nemours in Clermont, Florida. “A newborn doesn’t have a developed immune system and hasn’t yet received vaccines. Things like one sneeze from a stranger, a snotty little toddler running by the stroller, or even a grandma type in the baby’s face who doesn’t yet know that the next day she’ll be hit with the flu that’s cranking up in her body could all cause the baby to end up in intensive care with severe infection and possibly even meningitis causing permanent neurological damage at best and death at worse. Parents need to keep their newborns safely at home while their immune systems build.”

Not washing up after pumping gas
How many times have you stopped to sanitize or wash your hands after filling your car with fuel? “This is a small change that can make a big difference,” says emergency room nurse Lauren Mochizuki, RN. “Imagine all the different people that touch the pump every day. Now imagine taking all those germs, and ingesting them the next time you eat after you haven’t washed your hands! That pump can host a variety of different bacteria. S. pneumoniae and S. Pyogenes can live on inanimate objects for an extended time, and this is an easy way to contract strep throat or a respiratory infection.” We come into contact with more germs than we think; these are the 10 other things you should always wash your hands after touching.

Traveling unsafely
While public health experts say we should all be avoiding unnecessary air travel during the COVID-19 pandemic, there are some cleaning tactics you can use if travel can’t be avoided. Although air filtration systems on airplanes are more advanced than ever, and airlines are doing deeper cleaning between flights right now, “the seats can harbor all sorts of nastiness,” says Bryan. “Think about it, folks are trapped in a seat and their coughs, sneezes, mucus, food droppings, etc., all sit on the seat you’re about to inhabit.” Next time you fly, wipe down the armrests, tray table, and seat with a disinfecting or hand-sanitizing wipe before settling in, and read up on these 16 air travel rules you need to know for flying during the pandemic.
Sources:
- Karin Russ, MS, RN, clinical instructor at University of Maryland School of Nursing
- Lauren Bryan, RN, MPH, CCRN-K, CPH, CIC, an infection preventionist at UCHealth Yampa Valley Medical Center, in Steamboat Springs, Colorado
- Jeremy Hulsker, RN, CEN, Emergency Department Charge Nurse at UCHealth Memorial Hospital in Colorado Springs, Colorado
- Natalie Ingmire, MSN, RN, director of quality and patient safety at Centura Health at Avista Adventist Hospital in Louisville, Colorado
- Melissa Rubio, PhD, APRN, a nurse practitioner at the Lung Health Institute
- Valerie E. Rogers, PhD, RN, CPNP, assistant professor, University of Maryland School of Nursing
- Patsy Stinchfield, RN, vice president of the National Foundation for Infectious Diseases
- Terry Cralle, RN, clinical sleep educator and Saatva sleep consultant
- Ashley Wood, RN, BSN, a contributor at Demystifying Your Health
- Teri Dreher, RN, owner and CEO of NShore Patient Advocates
- Traci Powell, MSN, APRN, a neonatal nurse practitioner at Nemours in Clermont, Florida.
