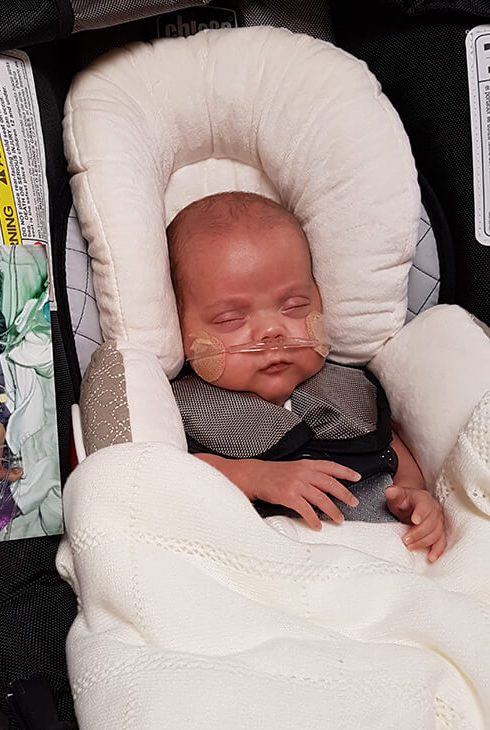
The first 23-week preemie to survive in more than a decade
A few years ago, we wrote about the miraculous survival of a baby born at 26 weeks. Now we have Samuel Rodriguez, born in April 2017 at just 23 weeks and 3 days, the result of a spontaneous placental abruption (separation of the placenta from the uterus). All Samuel’s mom, Jennifer Fresneda of Tioga, Texas, remembers is waking up to labor pains and rushing to the hospital, where she learned that her baby’s sole chance of survival was an emergency C-section. Sam actually took a breath upon emerging, but doctors immediately intubated and rushed him to the Neonatal Intensive Care Unit (NICU). When Jennifer and her husband were finally allowed to see their baby, Jennifer nearly collapsed from the shock. “He was the tiniest thing, hooked up to all these wires. I was frightened and powerless.”
Samuel spent four months in NICU, during which he had two surgeries, including surgery to correct a heart abnormality. On August 9, the day before his actual due date, Samuel was discharged from the hospital, a healthy baby boy, albeit with an apnea monitor and supplemental oxygen. “I didn’t even know babies so small could survive,” Jennifer marvels. Check out these 8 unsolved mysteries that still stump doctors.
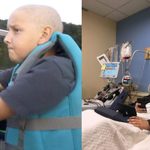
The boy who survived leukemia three times in ten years
Zach Swart was first diagnosed with acute lymphoblastic leukemia (ALL) in 2007 at age 6. Although ALL is generally highly treatable, Zach’s version played hardball. Zach’s first treatment consisted of more than three years of chemo. Two years later, the cancer returned. After another two years of treatment, Zach was deemed cancer-free. Then, when Zach was 15, the cancer came back. This time, chemo was just the pregame—to put Zach into remission in preparation for a bone marrow transplant (BMT). But three months later, after nearly dying from the side effects, Zach still wasn’t in remission. It seemed as if he was out of options when along came the miracle.
Kevin Curran, MD, at Memorial Sloan-Kettering Cancer Center in New York City, introduced Zach and his family to “CAR-T cell treatment,” which Dr. Curran developed through a research grant from St. Baldrick’s Foundation. It put Zach into complete remission in a matter of weeks. Within a month he received his BMT (from his brother, Ben). He’s getting stronger by the day. Read about the 10 parenting lessons we can all learn from children with cancer.
“I was initially afraid about CAR-T’s side effects,” Zach told Reader’s Digest. “But then I didn’t have any at all. I was so lucky, and it feels so good not to be sick anymore and to be home and see my friends. I’m determined to leave cancer far behind me.”
“Every day I see Zach smile, laugh, and just be a kid, it is truly a miracle,” his mom says. Find out 12 loving ways to support cancer patients.

Two parents’ lifesaving touch
On March 25, 2010, Kate and David Ogg heard the words every parent dreads: Their newborn wasn’t going to make it. Their twins—a girl and a boy—were born two minutes apart and 14 weeks premature, weighing just over two pounds each. Doctors had tried to save the boy for 20 minutes but saw no improvement. His heartbeat was nearly gone, and he’d stopped breathing. The baby had just moments to live. “I saw him gasp, but the doctor said it was no use,” Kate told the Daily Mail five years later. “I know it sounds stupid, but if he was still gasping, that was a sign of life. I wasn’t going to give up easily.”
Still, the Sydney, Australia, couple knew this was likely goodbye. In an effort to cherish her last minutes with the tiny boy, Kate asked to hold him. “I wanted to meet him, and for him to know us,” Kate told the Today show. “We’d resigned ourselves to the fact that we were going to lose him, and we were just trying to make the most of those last, precious moments.”
Kate unwrapped the boy, whom the couple had already named Jamie, from his hospital blanket and ordered David to take his shirt off and join them in bed. The first-time parents wanted their son to be as warm as possible and hoped that the skin-to-skin contact would improve his condition. They also talked to him.
“We were trying to entice him to stay,” Kate told the Daily Mail. “We explained his name and that he had a twin that he had to look out for and how hard we had tried to have him.” Then something miraculous happened. Jamie gasped again—and then he started breathing. Finally, he reached for his father’s finger. The couple’s lost boy had made it. “We’re the luckiest people in the world,” David told Today.
Eight years later, Jamie and his sister, Emily, are happy and healthy. The Oggs only recently told the kids the story of their birth. “Emily burst into tears,” Kate said. “She was really upset, and she kept hugging Jamie. This whole experience makes you cherish them more.” Read about these 9 nurses who went above and beyond the call of duty.

The church that cured one man’s cancer
It’s hard to say which was in worse shape: the run-down, century-old church or the cancer-ridden 56-year-old man perched on its crumbling steps. For years, Greg Thomas would sit on those very steps and pray when he walked his dogs along the country lanes in rural Minnesota. But in May 2009, he learned that the searing headaches, earaches, and jaw aches that had plagued him for the past year were due to inoperable head and neck cancer. Doctors told Greg’s family to be prepared to plan his funeral.
“I was sitting at the church one evening, pouring my heart out to God,” Greg told Reader’s Digest. “I kept looking at the building and the shape it was in. I said, ‘Before I leave this earth, Lord, I’d like to do something for you.’”
Greg decided that that something was to fix the peeling paint and the leaking roof, the mangled steps, and the rotting floorboards. He approached the church’s association with a deal: He would completely repair the building on one condition: “That I get a key to the front door so I can go in anytime I want to worship.”
Incredibly, as Greg scraped paint and replaced boards, he felt himself growing stronger every day. The more he worked on the church, the better he felt. As Greg continued to rehabilitate the church, medical scans revealed some startling news: His tumors were shrinking. Four years and 23 days after Greg’s diagnosis, his doctors were able to remove his feeding tube. Today Greg’s tumors are gone. He is considered officially in remission and no longer needs follow-up tests.
And the church? After five years of Greg’s labor and love, it has been restored to its former glory, too. Greg finished his main project last summer, but he will probably always be involved in maintaining its beauty (he still wants to replace some windows, for example). Greg held his third annual open house there near Christmas, inviting the entire community. “While I was restoring the church,” Greg says, “God was restoring me.” Be inspired by these 7 stories about the healing power of prayer.

The bladder cancer that saved a man’s heart
You might not consider a cancer diagnosis to be a miracle, but then you probably haven’t talked to David Shusterman, MD, a urologist who practices in New York City. Dr. Schusterman had a patient last year whose life was actually saved because of his cancer diagnosis (for privacy reasons, Dr. Schusterman can’t disclose the name of the patient). Here’s what happened:
Before any surgery, it’s protocol for a patient to get a presurgical workup, including blood tests and an EKG. In fact, before initiating any cancer treatment, the patient’s general health should be assessed. In this case, Dr. Schusterman explains, “We had a patient with bladder cancer, but when we checked his heart, we found a terrible heart condition.” The condition was so life-threatening that the patient was actually at risk of sudden death. Literally, as Dr. Schusterman told Reader’s Digest, “he was about to die of a heart attack.”
Because of the patient’s cancer diagnosis, his treatable heart condition was discovered in time. “He survived and was able to get his bladder tumor cured as well” and, in so doing, “beat two conditions that almost caused his death.” Find out the most miraculous recoveries these doctors have ever seen.

An internal tourniquet saves a man who was split wide open
By all accounts, Michael Cassidy should not be alive today. In March he was thrown from his motorcycle, face-forward, into a fire hydrant. The impact broke his pelvis wide open—literally, cracking him open like a book. It’s what Michelle McNutt, MD, chief of trauma at Memorial Hermann Red Duke Trauma Institute (MHRDTI), says is known as an “open-book fracture.”
When Michael arrived at the trauma center, Dr. McNutt had to make an immediate decision to utilize what’s called the REBOA (resuscitative endovascular balloon occlusion of the aorta) technique. It involves placing a flexible catheter into the femoral artery (located in the thigh), maneuvering it all the way up into the aorta (the main artery of the human body) and inflating a balloon at the end of the catheter. What this does is stop the blood flow beyond the balloon, which improves the person’s blood pressure and provides a sort of “bridge” to getting a severely injured patient into the operating room in time.
Another way of thinking about the REBOA is as an “internal tourniquet.” It’s revolutionary and the key to why Michael is alive today, according to Laura Moore, MD, FACS, an associate professor in the department of surgery at the University of Texas McGovern Medical School and medical director of the Shock Trauma ICU at MHRDTI. Michael was also lucky to have been where he was when the accident happened, or he might not have had access to REBOA. Amaze yourself with these 20 other true stories about luck.
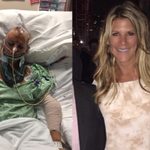
She’s alive and well, though half her skull is gone
In June of last year, Jennifer Beaver fell off a golf cart and landed on her head, leading to such a massive brain bleed that doctors had no choice but to remove half her skull to alleviate pressure. To say her prognosis was grim is an understatement. Colin Looney, MD, the orthopedic surgeon who helped repair Jen’s broken limbs, was also a friend of Jen and her husband, Bill. “I had operated on friends and neighbors before, but this would be my first time operating on a friend who was dying,” he recalls. “Talking to Bill shortly after, I tried to sound positive, but I’d seen so few patients survive massive brain trauma that I’m sure it all showed on my face.”
“So many things were going through my head,” Bill recalls. “One minute we’re having the best day. The next, all the doctors can say is ‘They’ll do their best.’ I just wanted to hold her hand and make it better. I couldn’t stand to think she’d never come home again.”
But she did go home again. After being brought out of a medically induced coma, Jen steadily improved. “Whenever I examined her,” Dr. Looney told Reader’s Digest, “I’d get emotional seeing how she’d improved beyond anyone’s hopes or expectations.” Read about what it’s like to be in a coma, from real-life survivors.
Jen, who’s back at work and is suffering no significant deficits, knows she’s a “walking miracle,” and she’ll be forever grateful to her doctors, including neurosurgeon Lola Chambless, MD.

She wasn’t supposed to live, let alone stand or dance again
Katie Vacek was never your typical high school senior: a class officer, sixth in her graduating class, a member of her school band, a varsity cheerleader, and, as if that weren’t enough, a member of the school’s powerlifting team. She’d planned to attend Texas State University in the fall until her future took a tragic detour in February 2017, when she fell 20 feet from a tree she was climbing while on a nature walk with friends and family. Katie landed facedown, but miraculously enough, she remained conscious. Turning over, however, she realized she couldn’t feel her legs.
Air-lifted to Memorial Hermann Red Duke Trauma Institute, Katie was found to have a fractured sternum, multiple broken ribs, a partially collapsed lung, and a broken spine. After a seven-hour surgery to fuse her spine, she was told she might not walk again.
But for Katie, it wasn’t enough just to have survived. Even if she’d never walk again, she was determined to stand beside and dance with her boyfriend at prom. That’s what she told her physical therapy team at TIRR Memorial Hermann, who came up with a plan and worked on their own time to fashion a harness for Katie and her boyfriend to wear together. A few weeks later, not only did Katie stand and dance beside her boyfriend at prom, but the two were also voted prom king and queen. Read on for 5 real-life miracle stories.

He’s alive because of his angels … and an AED
In January 2017, attorney Rand Mintzer, set out to complete his 25th marathon and his 11th Houston Marathon—but it didn’t go exactly as planned. “I wasn’t feeling great. I was struggling to keep up my pace, but I had heartburn and nausea. I even vomited on the sidelines,” Rand, 58, recalled. “Then I began feeling lightheaded, and my vision started to blur.”
At mile 15, he collapsed. He was in full cardiac arrest. Luckily, six spectators (aka Rand’s “angels,” as he calls them) who were trained in CPR ran to his aid. What’s more, he had collapsed right near an assisted-living facility that had an AED (a heart defibrillation device that saves lives). When the paramedics arrived, they transported Rand to Memorial Hermann Heart & Vascular Institute–Southwest, where Peter Chang, MD, positioned a stent to address a severe arterial blockage.
Today it’s Rand’s mission to encourage everyone to learn the miracle of CPR. “I will keep working to make sure that everyone who crosses my path knows CPR, so perhaps that percentage of survival will increase and someone else gets to go home to their loved ones.” Next up, read 13 more “unsolved mysteries” easily explained by science.
