How I Survived a Rattlesnake Bite—With No Way of Calling 911 or Getting to a Hospital
Updated: Jun. 30, 2022
There was no warning—just a silent and deadly bite in a remote area of Yosemite. And antivenom was 100 miles away.

Our son, Bridger, was two weeks old when my wife, Turin, and I decided to take a road trip. Two weeks later, we bought a 1988 Ford TransVan, a converted RV that we dubbed Queen, and left our home in Los Alamos, New Mexico.
I had grown up in Oregon, camping or hiking or canoeing every weekend with my parents and older brother, Garrett. At 33, I had worked as a wildland firefighter and as a filmmaker, traveling the world making adventure TV. I’d stepped on a deadly viper in Belize, been held up by guerrillas with AK-47s in the Democratic Republic of the Congo, and dodged a snapping crocodile in Papua New Guinea. Somehow loose bowels had been my worst affliction.
Turin’s lust for adventure matched mine. Since our wedding seven years before, she had taken 14 international trips, some for her work as a researcher at Los Alamos National Laboratory, but mostly for fun. Fun for her is rafting 145 miles through the Alaskan wilderness, which she did during her first trimester.

On our road trip, we shivered in Canyonlands National Park, went canyoneering in Utah’s San Rafael Swell, and surfed on the Oregon coast. Bridger wasn’t smiling yet, but we have photos of him in the West’s most spectacular places looking, as we interpreted his expressions, happy. He stayed that way until a few days before we reached Yosemite National Park, where we would meet up with my family on the last stop on our monthlong trip. Then he got a little colicky.
My brother has lived in El Portal, California, near Yosemite, for about seven years. Garrett manages the park’s vegetation—all 748,436 acres. His wife, Erin, is also a botanist. My recently retired parents had moved into their RV, which was parked in Garrett and Erin’s driveway when we arrived. We spent that first night passing Bridger around and telling stories. The next morning, April 23, broke warm enough to wear shorts, and Garrett suggested a family walk in the wildflowers above town.
“They’re peaking,” he said.
We climbed for three miles, through meadows and granite blocks, toward the 50-foot-high Foresta Falls. It felt like hiking through a Renoir. Garrett and Erin named off blooms of all colors, and we snapped pictures of the valley. At 11:45 a.m., we reached a bridge that crossed a waterfall. Bridger chirped his need for milk, and Turin stopped to nurse him.
Erin was the only one besides me who saw the snake. “Brown and big” is how she remembers it. I recall seeing a dust-red coil in new grass, but to me the snake was more of a sensation: a light tap just above the sock on my right ankle. Then I passed out.
When I awoke a minute or two later, and after I’d finished my first bout of violent vomiting, I heard my parents talking through the options to get me out. My mom had been an emergency room nurse and a physician assistant for 35 years. She and my dad had conducted some 700 missions as volunteers for the search-and-rescue team in Bend, Oregon. Neither had ever dealt with a rattlesnake bite.
I didn’t know it then, but the rule about rattlesnake bites is “time is tissue.” How many minutes or hours elapse before you get a dose of antivenom determines your fate: an afternoon in the ER if help comes quickly; amputation if a bite goes untreated for a few hours; or perhaps, in my case, death on a remote stone bridge.
We had no cell service to call for help, so Garrett took off running back toward El Portal, about three and a half miles away. He’d run about half a mile before he was able to call 911.
The dispatcher ordered a rescue helicopter and an ambulance, then asked Garrett to run about two miles to the town of Foresta, where he would meet the incoming paramedics and guide them to me.
I threw up every few minutes, in intensifying waves. Rivulets of blood, thinned by the venom, ran from the puncture wounds. My leg burned. I felt the same way I had after eating bad fish in Laos—except I was terrified.
“Get Bridger out of here,” I told Turin. I couldn’t stand the thought of them watching me die. She carried him down the road and watched from a distance as I gripped my parents’ hands.
Garrett had sprinted about a mile when he reached Crane Creek. But it was flooded, and the bridge was burned out except for four steel girders, each about eight inches wide and 45 feet long. They were wet and shaking from the thundering water 20 feet below. My brother isn’t reckless. He is calculating, confident, and experienced—all of which had little to do with why he decided to cross anyway. “You were actively dying,” he told me later. So he sat down on one of the girders and scooted across. He ran more than two miles in 19 minutes. That included the bridge crossing.
Within minutes of Garrett’s 911 call, Jason Montoya, a Yosemite park ranger who specializes in technical rescues for the elite Yosemite Search and Rescue, was in an ambulance speeding my way. To be safe, he’d ordered a second helicopter equipped with a hoist to get me out of the canyon, plus a team of volunteers to hike up from El Portal.
Based on the coordinates Garrett gave to dispatch, Montoya figured they’d need to fly me out of the canyon on the hoist-equipped helicopter, then transfer me to the rescue helicopter, which had a paramedic on board. Best-case scenario, he thought, I’d be in the emergency room in an hour and a half, which might mean I’d get to keep my leg.
During the busiest times of the year, there’s a hoist-equipped helicopter stationed in Yosemite. But it wasn’t scheduled to arrive for another week. Dispatch tried its usual backup, but it was on another call. A second backup was sidelined with an oil leak.
Just below Foresta, Garrett crossed back over Crane Creek on an intact bridge and met the ambulance. A fallen tree had blocked its path, and one wheel was stuck in the road’s soft shoulder. The medics were scrambling to pull gear from the truck: IVs, an inflatable backboard, drugs, and other medical supplies. Garrett, Montoya, and two medics took off running with a bag of medical equipment. But when they reached the burned-out bridge, Montoya insisted they turn around rather than scoot across the girders as Garrett had done.
“We couldn’t take that risk,” Montoya says. Instead, they ran more than a mile back up the hill they’d just descended and crossed on the upper bridge. Then they bushwhacked toward me across cliffs and through a half mile of waist-high poison oak.
When they arrived, I was pale and sweating, moaning in pain. My mom and dad had been rolling me from my back to my side to vomit or defecate. My blood, unable to clot, wept from the puncture wounds on my ankle. Bruising, a sign of internal hemorrhaging, had bloomed to above my knee.
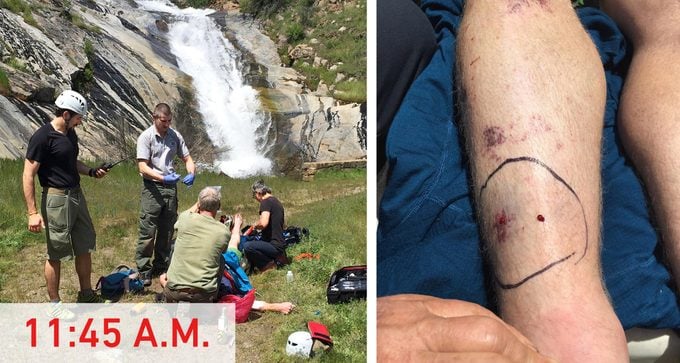
One of the medics, Levi Yardley, ripped open his medical kit. During the summer, Yosemite stocks a small supply of antivenom, but the supply hadn’t yet been restocked. Instead, he tossed my mom a blood pressure cuff and grabbed 1,500 milliliters of saline, a pill to stop the vomiting, and fentanyl, a powerful opioid painkiller.
My mom, the ranking medical professional on the scene, drew the drugs into syringes. But when Yardley asked her to start an IV, she paused. “I don’t feel comfortable doing that,” she said. “I’m a PA, but I’m a mom first.”
So Yardley stuck a 16-gauge needle—essentially a medical railroad spike—into each of my arms. The drugs worked. I hurt less and stopped purging, and the IV rehydrated me.
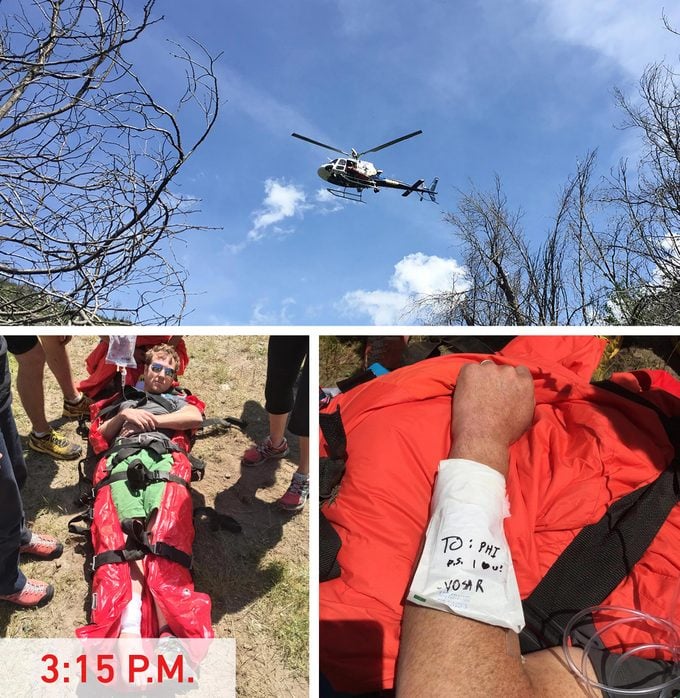
Finally, at 1:11 p.m., approximately 80 minutes after I was bitten, a helicopter took off from Paso Robles, an hour and 45 minutes away. The team from El Portal loaded me onto an inflatable backboard, and I mustered a smile when they put aviator sunglasses on me to protect my eyes. We even snapped a family photo, with Turin, Bridger on her chest, giving a thumbs-up and me looking like smiling death. When the helicopter was 20 minutes away, the team carried me to the helicopter pickup point.
“If we don’t get him out of here now, we’re going to have a critical patient on our hands, and I don’t have the meds to deal with him,” Yardley told Montoya. The drugs had run their course, and my symptoms had returned. Then a bee stung my thigh. Panicking, I told them I was allergic. Yardley told somebody to get an EpiPen.
“Please don’t,” I pleaded, afraid the epinephrine could agitate the snake venom. Yardley gambled that if I hadn’t gone into anaphylaxis yet, I wouldn’t.
As the brush beat about in the copter’s downdraft, a cable was lowered about 200 feet. I felt myself tugged up from the ground, and a surge of relief.
As the thumping of the helicopter faded, Turin finally gave in to the dark thoughts she’d been ignoring for the past three hours. She and my parents broke into sobs. Bridger didn’t make a sound. He hadn’t—not a single colicky cry—since the bite.
Bill Hayes keeps a collection of snakebite kits in a display case outside his office at Southern California’s Loma Linda University, where he is a biology professor and one of the country’s leading authorities on snakebite treatments. There are dozens of kits. Some contain razors to cut the wound and let the venom leech out. Others have pumps to suck a bite dry or sulfide to sterilize it. That day in Yosemite, we didn’t have one of these kits, which is probably just as well. None of them work. Nor do any of the folk treatments people still try today, which include freezing the wound and slathering it with motor oil. Know these tips to save your own life in 12 scary emergencies.
“Antivenom—that’s the only cure,” Hayes told me when I went to see him six months after I was bitten.
Today’s antivenom isn’t so different from what French scientist Albert Calmette developed in the 1890s while working in Vietnam. When a flood pushed dozens of cobras into a nearby village, 40 people were bitten and four died. Calmette, who was a protégé of Louis Pasteur, applied the same techniques his mentor was using to produce vaccines for rabies and anthrax. He milked cobras and injected tiny amounts of venom into horses. After a few weeks, Calmette extracted the horse blood and spun out antibodies that targeted cobra venom.
Snakebites killed more people back then, but the World Health Organization still considers them a global health crisis. Each year, snakes kill more than 81,000 people and maim hundreds of thousands more. Modern antivenom is still made in livestock, and while it has gotten more effective over time, it is mostly species-specific.
In the United States, it’s also outrageously expensive. A single vial can cost $18,000, and most victims require four to six vials. Many clinics and hospitals don’t stock it, and it’s rarely carried by search-and-rescue teams.
After the helicopter touched down at Doctors Medical Center of Modesto, nurses wheeled me into the emergency room and cut off my shorts and T-shirt, then hooked me up to my first IV laced with antivenom. Five and a half hours had passed since my bite. Over the next 72 hours, I’d receive 18 vials of the lifesaving antidote.
Each of the half-dozen doctors I saw told me that this was either the first snakebite they’d ever seen or the worst. Poison Control guided my care. My leg, from toe to hip, turned black and yellow and eventually swelled to more than twice its normal circumference. During my first day in the hospital, I received morphine every two hours, yet the pain remained too severe for me to sleep. It felt as though nerves were popping in my leg.
The orthopedic surgeon grew convinced that I had developed compartment syndrome, a side effect of swelling that cuts off circulation to extremities and in the worst cases leads to amputation. Fixing it would require an only slightly less intrusive emergency surgery—deep incisions along the length of my leg to relieve the pressure.
My night nurse, John, was a 71-year-old Vietnam vet who’d been bitten twice by rattlesnakes. He joked that I should have done what he did to survive: eat the snake that bit me. (“More gamy than fishy,” he said.) It was John who saved me from going under the knife. In the early morning, he found a pulse at the top of my foot, a sign that I still had circulation, which was enough to keep the surgeons from operating.
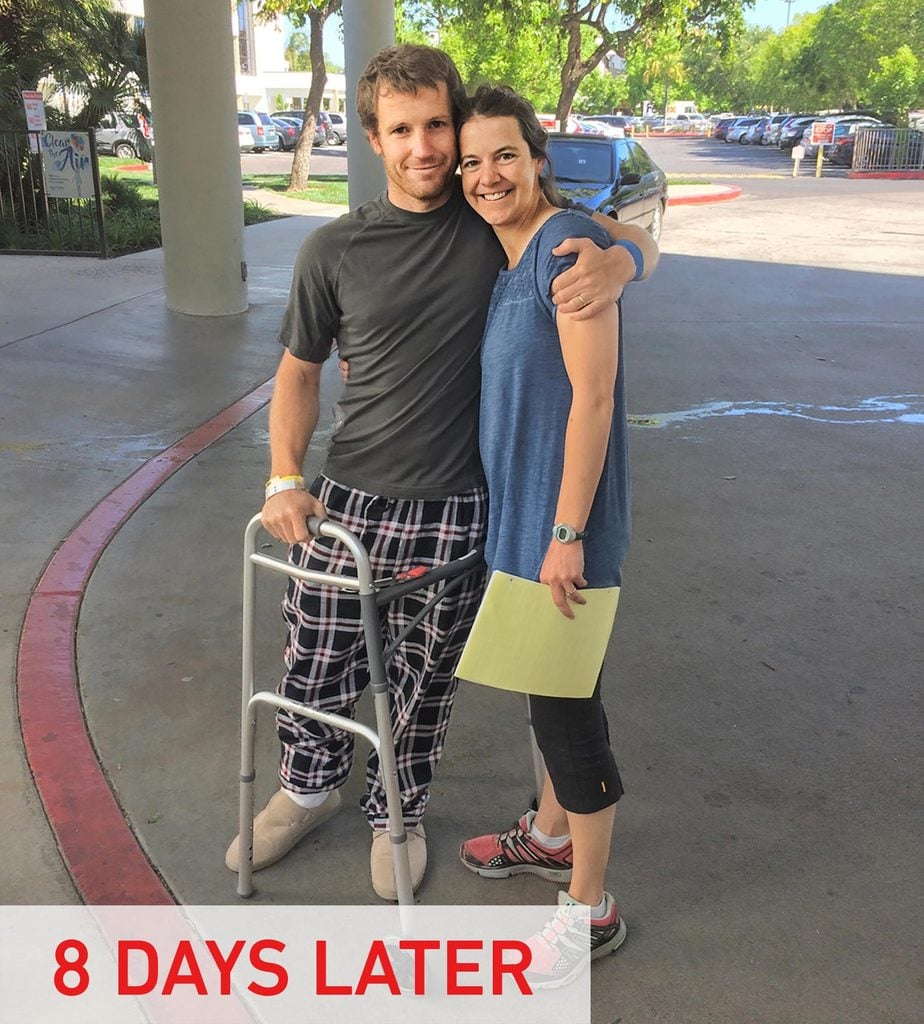
It took four days for me to move from a bed to a chair. Two more to stand up. And eight before the doctors released me. Until then, Turin, Bridger, and my parents stayed in Queen in the hospital parking lot. After I was released, it took a month for me to walk normally and six months for the swelling in my leg to go down.
In search of some kind of closure, the following September, Garrett and I revisit the bridge where I was bitten. This time we’re joined by Robert Hansen, who edits the journal Herpetological Review, and Rob Grasso, a Yosemite park ecologist. We find the pair, dressed in safari gear, flipping over rocks and logs with a rake.
Garrett and I strap on protective Kevlar chaps, as though we’re preparing to disarm a car bomb. Hansen rolls his eyes when he sees us.
“They don’t want to bite you,” he says, then wades deeper into the oak trees, where he thinks he has heard the high-pitched zzzt of a baby snake’s rattle.
We’re here because the snakebite did more than scar my ankle. I feel fine physically but have been consumed with an unfamiliar sense of vulnerability. To be snakebit also means to experience a period of bad luck, which is what I’ve lived through since the ordeal. Shortly afterward, our dog Mud got hit by a car. He survived, but weeks later we had to put down our other dog, 13-year-old Lucy. A friend sustained a severe concussion while we were biking. Another broke his neck skiing. Yet another lost his dad to a stroke.
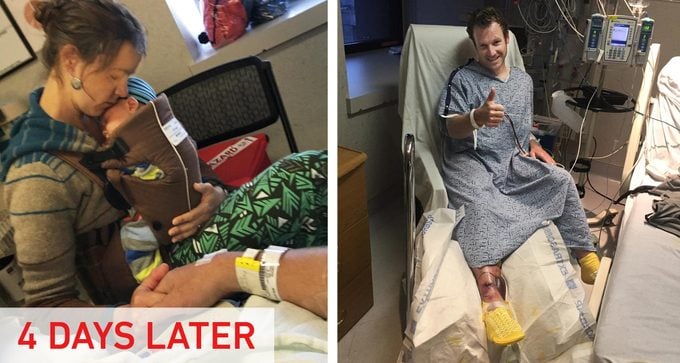
Plenty of good happened too. That I lived comes to mind. Waking up to Bridger every day. My parents bought a house near our home in Los Alamos to be closer to us. But I felt broken. Fear was no longer thrilling—just scary and everywhere. At night, I’d grab Turin in my sleep because, I insisted, she was falling and I needed to catch her. I struggled to walk in the woods without seeing something slither.
“Maybe you just see the world like the rest of us always have,” one friend suggested.
Maybe, but I miss my old optimism. Instead, I feel sad, grateful, dazed. I want to know whether I did something wrong to deserve my fate. Maybe I violated some rule of nature unknown to me. Maybe the bridge would reveal answers only the herpetologists can interpret.
Rattlesnakes, Hansen tells me, emerge in spring hungry, spend their summer hunting, and head back to the same den in the fall to breed. Hansen and Grasso suspect that I was bitten after stumbling onto a den during spring emergence.
Finally we reach the bridge, the exact spot where I was struck. I’d always thought of rattlesnakes as the gentleman’s viper—considerate enough to warn you before they bite. Mine never rattled. I ask Grasso why, and he says he’s not sure.
Because the creek had been flooded at the time, he posits, the snake’s senses might have been overwhelmed by tremors of rushing water shaking the bridge. It was probably hunting and unaware of me until I stepped into its field of vision and boom!
“I’m surprised you lived,” Grasso says. Which I hear as “You’re lucky to be here.”
“That ledge there, that’s my best guess,” Hansen says, pointing to a shadowy overhang located about 30 feet up a slab of sloping granite, where he imagines the den might be.
Garrett turns to me. “Want to check?”
“Yeah,” I say, trying to sound bold. When we reach the ledge, I peer into a dark crack and see a mouse skitter across the base of the opening, but no snakes. And I feel very lucky indeed.