11 Signs You May Have Already Had COVID-19
Updated: Nov. 24, 2022

You felt lousy, you had trouble breathing—did you have COVID-19? Here's what the experts say you should look for if you think you've been infected.
With all the reports about the spread of COVID-19, are you looking back and wondering if that flu-like illness you had in mid-February was actually the novel coronavirus? If so, you’re not alone—and yes, you could have had it.
The COVID-19 outbreak began in Wuhan, Hubei Province, China. So far, there have been more than 5.6 million documented cases of the respiratory illness confirmed around the globe, according to Johns Hopkins University. The first confirmed case in the United States was on January 20, 2020, in the state of Washington, according to a case study in the New England Journal of Medicine. The first documented “community spread” in the United States happened in late February. Community spread refers to a COVID-19 diagnosis in someone who did not travel to countries with the virus or come into contact with a known sick person, according to the Centers for Disease Control and Prevention (CDC). But researchers have since found deaths from the virus in areas of the country far from Washington state that occurred well before community spread. What this all means is the virus was circulating before we realized it, and most likely more people have been exposed than anyone thought.
Here are 11 silent signs that you may have been infected with COVID-19 and what you can do about it now. (Spoiler alert: Get an antibody test.)
COVID-19 sign: You were really sick in February
If you were sick before January, it likely wasn’t COVID-19, says Adam Spivak, MD, an infectious disease doctor at the University of Utah in Salt Lake City. “COVID-19 was likely here earlier than we thought it was,” he says. “If you were sick from mid-January to mid-February, it’s possible you had COVID-19. This timeframe is key.” Widespread testing wasn’t readily available during this time so you likely wouldn’t have known.

COVID-19 sign: Your fever and cough weren’t the flu
You were so sick. You had a fever for days, a hacking cough, and were exhausted, but your flu test was negative. It could have been COVID-19, Dr. Spivak says, noting that flu season and the COVID-19 pandemic overlapped. “If you weren’t tested at the time or you were negative for other tests such as the flu that were available, it could have been COVID-19,” he says. “There is so much overlap with colds or flu and coronavirus symptoms, which is why testing for COVID-19 has been so emphasized.”
COVID-19 sign: You suddenly lost your sense of smell or taste
This seems to be a hallmark of COVID-19 infection, but it’s not a slam dunk by any stretch, says Benjamin Singer, MD, an assistant professor in pulmonary and critical care at Northwestern University Feinberg School of Medicine in Chicago. As many as 64.4 percent of people with COVID-19 report a loss of smell or taste, according to an April 2020 study in the Journal of the American Medical Association (JAMA). The CDC recently added loss of taste and smell to the list of possible Covid-19 symptoms. “Reported loss of smell and taste appear more commonly with COVID-19 than other respiratory viruses, but other viruses and non-infectious entities like allergies can cause these same symptoms,” says Dr. Singer.
COVID-19 sign: Your loved ones were infected
Many people who are infected with this virus have mild or no symptoms, says Dr. Singer. This means you could have had coronavirus and not had a clue.”If you were around people with confirmed cases, you likely have been exposed and may have been one of the people who don’t develop any noticeable symptoms.” This may also be true for people who work in the healthcare system and treated people for Covid-19.
COVID-19 sign: Your toes were a mess
“Covid toes” are a thing, Dr. Singer says. They are marked by purple or red, itchy wounds. “Skin manifestations, particularly of the toes, could be something that makes people who weren’t tested look back and say ‘was that a manifestation of COVID19?'” he says. But he cautions that toes with this appearance aren’t a telltale sign of COVID-19, as there could be other causes. If you are concerned, talk to your doctor.

COVID-19 sign: You had chills, muscle pain, or a sore throat
As doctors learn more about COVID-19 and how it behaves, the CDC has been adding to its symptom list. Other symptoms that could suggest COVID-19 include chills, repeated shaking with chills, muscle pain, headache, and a sore throat.
COVID-19 sign: You noticed a strange rash on your child
There have been concerning reports of rashes and multisystem inflammatory syndrome in children (MIS-C) who had the virus, the CDC states. Other signs of MIS-C include fever, abdominal pain, vomiting, diarrhea, neck pain, and feeling tired. Call your doctor if you notice any of these signs in your child, the CDC notes.
COVID-19 sign: Your stomach was acting up
Coronavirus is a respiratory illness, but not everyone experiences coughing or shortness of breath. For some, diarrhea may be the first and only sign of COVID-19, according to a March 2020 study in The American Journal of Gastroenterology. Researchers suggest that people with new-onset digestive symptoms such as diarrhea who may have been in contact with individuals infected with COVID-19 should have a high index of suspicion.
COVID-19 sign: You have cancer
People who live with cancer have a 60 percent higher risk of testing positive for COVID-19, according to a May 2020 study preprinted in medRxiv from Massachusetts General Hospital, sponsored by Stand Up 2 Cancer. This risk was higher among participants older than 65 years of age and among men. What’s more, people with cancer were more likely to have severe cases of COVID-19 that required hospitalization.
COVID-19 sign: You had a stroke out of the blue
There’s a link between COVID-19 and stroke risk—even among younger patients. Here’s what doctors and researchers know so far about stroke risk and coronavirus.
COVID-19 sign: You woke up with pink eye
Pink eye infection, or conjunctivitis, may be a sign of coronavirus, but this is very rare, according to the American Academy of Ophthalmology. They advise if you develop pink eye, do not panic. “Call your ophthalmologist to let them know and follow their instructions for care,” the Academy suggests. These are the places you’re most likely to catch COVID-19.
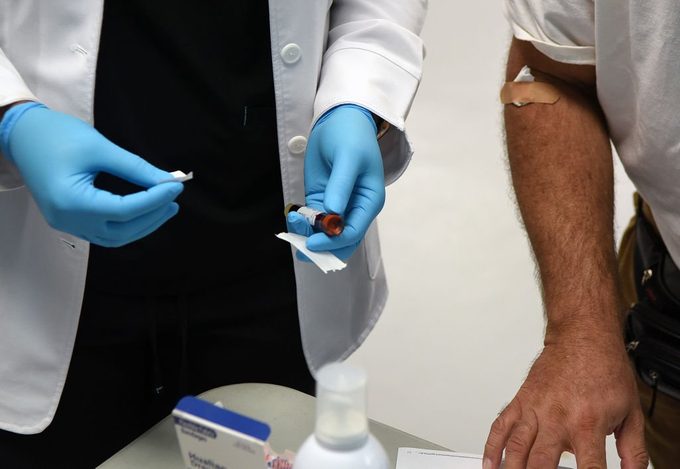
The role of COVID-19 antibody testing
The real question is what to do if you think you may have had COVID-19. When in doubt, seek antibody testing, experts agree.
The only way to know whether you have had COVID-19 is to be tested for antibodies, says Matthew G. Heinz, MD, a hospitalist and internist at Tucson Medical Center in Tucson and former director of provider outreach in the Office of Intergovernmental and External Affairs, a part of the U.S. Department of Health and Human Services, under the Obama administration. Antibodies are produced when the body mounts its immune response to an infection, according to the Food and Drug Administration. Antibody tests can tell whether someone has been infected with COVID-19 in the past as opposed to having an active infection, the agency notes.
Antibody testing is not fail-safe and no-one can say for sure that you can’t get COVID-19 twice, Dr. Heinz says. “These blood tests can say if you have had COVID-19 but we don’t know if the presence of antibodies means you are immune and if so, for how long this immunity may last.”
Time it right, he advises. Don’t get tested too soon after symptoms as that could lead to a false-negative result. You don’t need to have had symptoms to consider testing since many people don’t experience any symptoms. “If you are even asking the question, ‘did I have COVID-19,’ order the test,” he says. “The more we know about how many people have had exposure, the better.” This information can let researchers know how close we are to “herd immunity.” This means that a high percentage of people in the community are immune to a disease so its chances of spreading from person to person are unlikely, according to the Association for Professionals in Infection Control and Epidemiology. Next, find out what a coronavirus survivor wants you to know. And if you’re wondering, is the pandemic over? Here’s what experts have to say.
Sources
- Johns Hopkin’s University: “COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU)”
- New England Journal of Medicine: “First Case of 2019 Novel Coronavirus in the United States”
- Centers for Disease Control and Prevention: “CDC Confirms Possible Instance of Community Spread of COVID-19 in U.S.”
- Adam Spivak, MD, an infectious disease doctor at the University of Utah in Salt Lake City
- Benjamin Singer, MD, an assistant professor in pulmonary and critical care at Northwestern University Feinberg School of Medicine in Chicago
- JAMA: “lterations in Smell or Taste in Mildly Symptomatic Outpatients With SARS-CoV-2 Infection”
- CDC: “Symptoms of coronavirus”
- CDC: “For Parents: Multisystem Inflammatory Syndrome in Children (MIS-C) associated with COVID-19”
- The American Journal of Gastroenterology: “Digestive Symptoms in COVID-19 Patients with Mild Disease Severity: Clinical Presentation, Stool Viral RNA Testing, and Outcomes”
- medRxiv: “Cancer and risk of COVID-19 through a general community survey”
- American Academy of Ophthalmology: “Eye Care During the Coronavirus Pandemic”
- Food and Drug Administration: “Coronavirus (COVID-19) Update: Serological Tests”
- Matthew G. Heinz, MD, a hospitalist and internist at Tucson Medical Center, Tucson and former director of provider outreach in the Office of Intergovernmental and External Affairs, a part of the U.S. Department of Health and Human Services in the Obama administration
- Association for Professionals in Infection Control and Epidemiology: “Herd Immunity”

