Why Fully Vaccinated People Everywhere Still Need Masks Indoors
Updated: Sep. 01, 2023

The CDC recommends that vaccinated people almost everywhere wear masks in indoor public places. Here's why it's a good idea.
Keeping up with COVID-19 updates
Thanks to the rapidly spreading Delta variant and waning immunity from earlier vaccines, it’s still mask season in the United States—even for fully vaccinated people located in just about any part of the country.
“The guidance in this situation and evidence that we have about mask-wearing has really evolved as the Delta variant has taken off,” says Jennifer Balkus, PhD, assistant professor of epidemiology at the University of Washington School of Public Health. “[Masks are] an incredibly important and easy and accessible tool to use. There’s no doubt about their efficacy.”
The Centers for Disease Control and Prevention (CDC) recommends that fully vaccinated people wear masks in public, indoor settings only in areas of the country with “substantial or high transmission” rates.
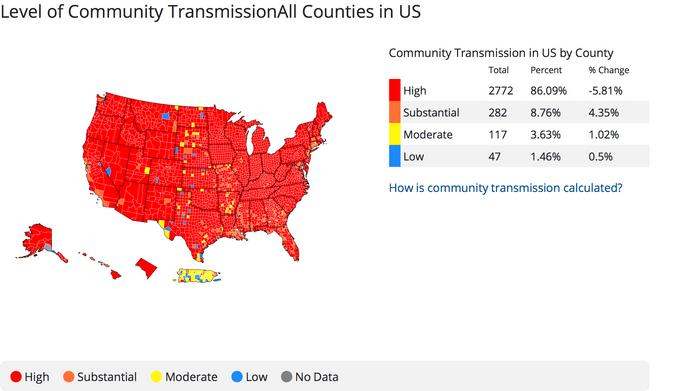
However, 96.3 percent of the country is now considered to have a substantial or high transmission rate, according to the CDC’s Covid Data Tracker (as of October 11, 2021). That means that effectively if you are fully vaccinated, you should be wearing a mask in indoor public places no matter where you are located.
The mask recommendation never went away for people who are unvaccinated, so if you are not vaccinated and age 2 or older, you should be wearing a mask in indoor public places.
Here’s what we know right now about mask-wearing for fully vaccinated people. Plus, find out why you shouldn’t share photos of your vaccine card.
COVID-19 is still very much a threat
Case counts are going down, but due to the Delta variant, they’re still higher than they were at any other point in the pandemic besides last winter’s peak. Areas with higher percentages of unvaccinated people like Florida, Mississippi, and Tennessee saw the worst of the recent surge.
More COVID-19 hospitalizations occurred this Labor Day than last year. The healthcare system in Alaska is so overburdened that officials are now rationing care.
To date, about 44.5 million people in the United States have been infected with SARS-CoV-2, the virus that causes COVID-19.
Even vaccinated people can get infected
The three existing COVID-19 vaccines are still effective against the Delta variant, but not quite as effective as they are against the original strain of the virus.
That means you can get infected and sick even if you’ve had your one Johnson & Johnson shot or your two Pfizer or Moderna shots. These are called breakthrough infections. (You’re considered fully vaccinated two weeks after your last COVID-19 inoculation.)
And while breakthrough infections are usually relatively mild in vaccinated people compared to infections in unvaccinated people, they can be serious. “Breakthroughs are still a concern,” says Ravina Kullar, PharmD, a fellow of the Infectious Diseases Society of America and adjunct faculty at UCLA David Geffen School of Medicine. “I’ve seen breakthrough infections where people have been hospitalized, and we still don’t know the risk of post-Covid complications.”
Infected vaccinated people can spread the virus
Anyone who tests positive for COVID-19, vaccinated or unvaccinated, can still transmit the virus. This is true whether or not you have symptoms, says Dr. Kullar. And Delta is way, way more infectious than the earlier strain.
The number of viral particles in an infected person’s nose and throat is more than 1,000 times higher with Delta. Higher viral load means easy spreading.
By one estimate, you only have to be in contact with a COVID-19 infected person for one second to get infected yourself, says Dr. Kullar. You should be especially careful in these places you’re most likely to catch Covid.
The vaccine doesn’t fully protect some people
The vaccines don’t work equally well for everybody. People who have weakened immune systems because they take immunosuppressive drugs after an organ transplant, are undergoing chemotherapy, have HIV/AIDS, or have another condition don’t get as much protection. That’s why the Food and Drug Administration authorized in August a third dose of Pfizer or Moderna for people in this category.
If you are positive for SARS-CoV-2, no matter vaccination status, you could infect someone who has a higher chance of becoming severely ill.
The vaccines become less effective over time
Emerging evidence also indicates that vaccine effectiveness is waning as time passes, says Dr. Kullar.
This is why the White House announced its intention to start boosters in September on a rolling basis eight months after the first round. In September, the FDA authorized a booster dose of the Pfizer-BioNTech vaccine for those who meet certain criteria.
And don’t forget, the vaccine is not authorized for anyone under the age of 12.
Masks are effective
Multiple studies confirm that masks work to slow COVID-19 infections. No one knows exactly how much, but research indicates the reduction could be as high as 70 percent, 80 percent, or higher.
“The fit of the mask is key, even with a cloth mask,” says Dr. Balkus. That means “ensuring that it’s fitting snugly on the bridge of your nose and under the chin. Not having big gaps is important.”
Surgical and N95 or KN95 masks are good but aim to have at least two layers of fabric cotton or cotton blend, says Dr. Balkius.
“It should be breathable without gaps around the nose and chin,” she says. “What’s comfortable for you is the biggest thing.” You may have to wear them for more than a few minutes.
While surgical masks are disposable, cloth masks are washable, says Dr. Balkus. Ideally, you would wear a new surgical mask in every new mask setting and wash cloth masks after each use. The reality may not be that simple.
“Trying to find that practice balance is the key thing and making sure you’re wearing it,” says Dr. Balkus. Next, learn more about what a post-COVID life could look like.




